Combat Arts Ankle Injuries Overview

The ankle joint is composed of two separate joints that combine to create the ankle joint or ankle complex. The complexity of the ankle structure allows heavy weight loads to be carried and conducted through a small area without harm.
Part of how the ankle structure succeeds in doing this is through the four strong ligaments, tendons, including the Achilles tendon, and 20 muscles that hold the foot together and keep its shape. The ankle joint is a very complex area that is placed under tremendous pressure by the weight of the body when standing or in motion.
Ankle Injury Causes
Ankle injuries are commonly defined as a sports injuries. Combat athletes can turn an ankle just stepping of the tatami ackwardly. A simple round-house kick delivered to an uneven body part can cause a painful, debilitating injury. When the body is standing or walking the ankle supports the body’s weight. When the body is running the ankle will support up to thirteen-times the body’s weight.
Carrying that weight and pressure is possible by the complex way the ankle is put together, which places over 80% of the weight load on the tibiotalar joint, with the last approximately 17% supported by the fibula.
The talar dome carries most of the load on the tibial-talar joint, up to 90%, with the rest distributed across medial and lateral surfaces. This weight distribution reduces pounding on any one area and allows weight to be dispersed correctly over all parts of the ankle complex. The ends of all bones are also protected by articular cartilage, and the space between bones within the joint contains a thin liner called the synovium that releases synovial fluid, a lubricating protective fluid that ensures fluidity, ease of movement, and prevents bone, ligament, and tendon friction.
The complexity of the ankle joint also means there are many ways that the ankle may be injured, and ankle injuries are one of the most common reasons for seeking medical aid.
Symptoms of Ankle Injury

Types of Ankle Injuries
Since the ankle joint is a hinge joint where the tibia, fibula, bones of the foot or talus participates, some several ligaments and tendons are prone to injury. These include the sinus tarsi syndrome, ankle fracture, posterior impingement syndrome, and Achilles tendon rupture.
Is that Pain a High Ankle Sprain, a Ligament Tear, a Fracture or Hematoma?
Get our Performance and Lifestyle Newsletter to Keep Learning and Growing.
Related Injuries
STS Is an acute ‘whiplash’ type of injury occurs to the subtalar joint, usually after a jump, fall, or abrupt stop. STS may occur after the martial artist has experienced many traumatic ankle injuries involving inversion and/or supination which have left the area weakened and more susceptible to injury.
Sinus tarsi syndrome also occurs when the subtalar joint is unstable because of biomechanical or alignment issues that make it easier to injure. This is one of the most common causes of the sprained ankle that won't heal. It may have mild or severe symptoms. Martial artists can usually train around symptoms if the injury is mild. While it can be difficult to discern this problem on an X-ray or MRI, a physical therapy or dance movement specialist will be able to properly diagnose it.
Symptoms
This injury can be difficult to catch and diagnose in the early stages since the injury occurs deep inside of the ankle, and symptoms may take time to develop. Basic symptoms associated with STS include:
Causes
Martial artists may incur STS when doing moves that include jumping, kicking, throwing, or other executions that sprain the talocrural joint or injure the subtalar joint. The martial artist can often continue training around this injury if it is mild.
To learn how Sinus Tarsi Syndrome is diagnosed Click Here
A broken ankle may occur in an injury along with a sprain and/or strain. It can be extremely difficult or impossible to diagnose a broken or fractured ankle instead of only a strain or sprain without an X-ray. A broken ankle means any one of the three bones which comprise the ankle has been fractured or broken, typically from an acute injury.
Symptoms
Many basic symptoms may be observed separately or together when an ankle bone has been broken. Many of these symptoms are also seen when an ankle is sprained or strained. That is why it is essential to have an X-ray of the ankle if there is any possibility of a broken bone to ensure proper care. Symptoms may include:
Causes
The martial artist who performs a flying judo kick and lands on an ankle instead of rolling out may appear to have sprained or strained an ankle but may have broken or fractured it.
To learn how Ankle Fracture is diagnosed Click Here
The peroneal tendons are a set of two tendons essential for preventing ankle sprains and rollovers. These two tendons work in tandem, one is longer, one is shorter, and they both run parallel down the outside of the ankle.
These weakened or damaged tendons may not regain strength on their own after being injured. Symptoms of peroneal injury include
Peroneal tendons may fray and deteriorate when repeated spraining causes tiny tears or longitudinal rips in the tissue. Damage of this type causes tendons to develop inflammation which increases irritation to tendon sheaths that surround and protect them. Peroneal tendon weakness may occur after rolling the ankle during BJJ grappling when going for a takedown and damage could occur if the ankle is repeatedly injured without treatment.
To learn how Peroneal Tendon Weakness and Damage are diagnosed Click Here
This occurs when the martial artist experiences pain at the back of the ankle, tenderness, or aching while doing kicks and actions that point the feet including jumps, squats, kicks, or other training activities, and during rest. It can also result from a previously sprained ankle that was not correctly rehabilitated.
Primary symptoms will include:
Posterior impingement syndrome is the result of extreme ankle compression while foot and ankle are pointed away from the body, creating pressure on the bone or soft tissue that results in damage and pain in the back of the ankle. It may result from a previously sprained ankle that was not correctly rehabilitated. Martial artists may get this injury while doing high kicks and tornado kicks and landing incorrectly when thrown.
To learn how Posterior Impingement Syndrome are diagnosed Click Here
The Achilles tendon runs from the bottom of the calf muscle to the back of the heel bone and requires immediate treatment if injured to prevent the possibility of a worse injury occurring from complications.
Achilles injuries may occur during fight events while doing takedowns, or from fast stops, starts, and quick side movements when sparring. This type of injury typically results from repetitive overuse during training and events. Other possible causes include sudden changes in training such as drastically increasing the intensity and/or time spent training, wearing unsupportive footgear, high foot arch with tight Achilles tendon, flat or overpronated feet, hard training surface, or suddenly changing from training on the grass to a harder surface such as a track, running up and down hills, or uneven body strength such as weak feet with very strong calf muscles.
To learn how Achilles Tendon Rupture are diagnosed Click Here
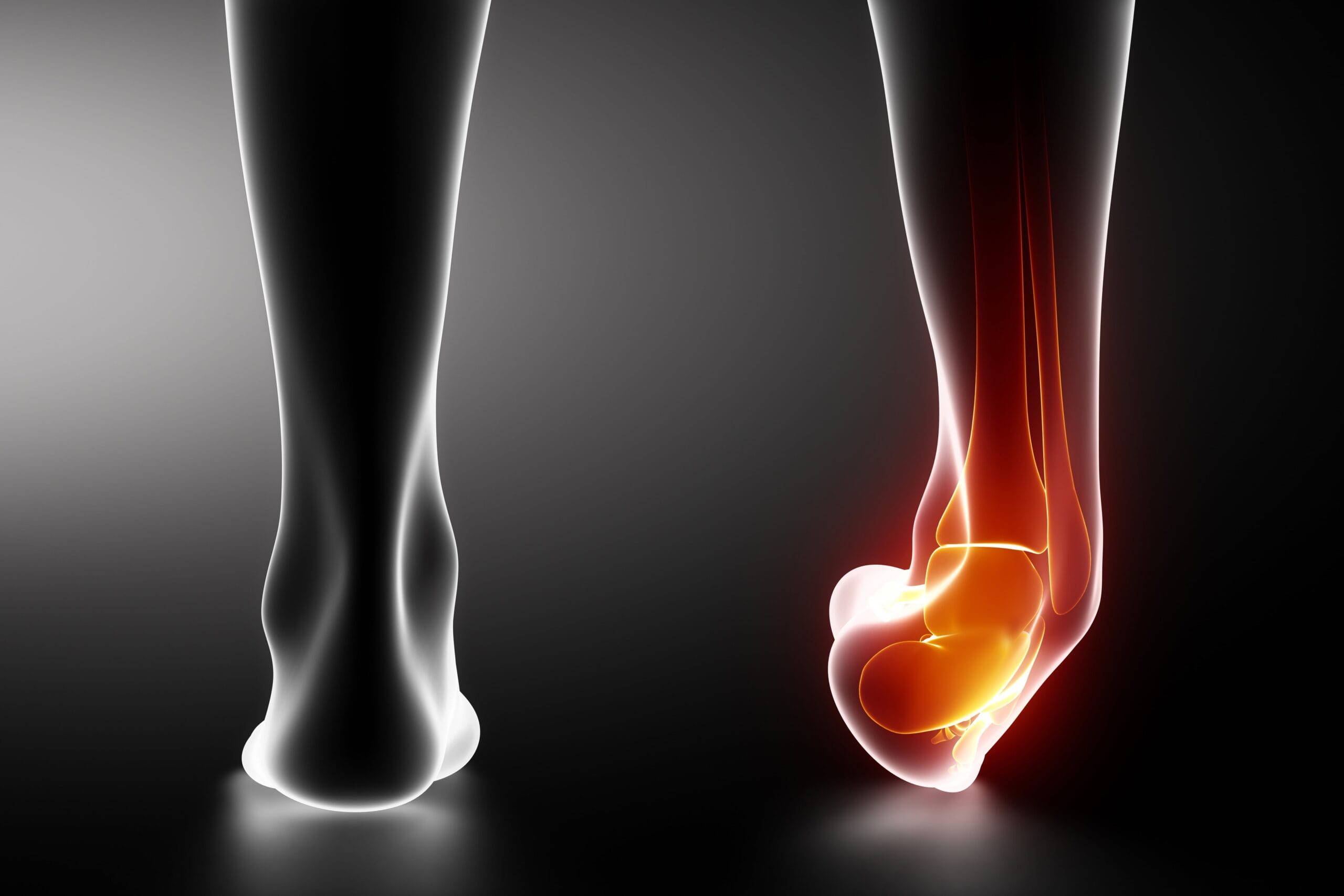
Common Injuries
Learn more about common ankle injuries such as ankle strains and tendinosis in our Common Injuries section.
Ankle Injury Diagnosis
The diagnosis of ankle injuries is done via physical exam and imaging. Imaging forms the mainstay of diagnosis as it allows the assessment of the tendons, ligaments, bones, and muscles in the joint. Blood tests are not as helpful and are not used to diagnose ankle injuries.
Injury Specific Diagnosis
Physical Exam
The talocrural joint is checked before the subtalar joint. Anterior and posterior glides of the talus on the tibia are seen. A talar tilt test is recommended for assessing talocrural joint stability. Mobility of the contralateral ankle and foot joints are also assessed.
The stability of the subtalar joint is examined with medial and lateral subtalar joint glides. This is done by gliding the calcaneus over a stabilized talus. It is performed in the transverse plane with subtalar joint distraction. Another stability test is done with the athlete lying supine. The ankle is dorsiflexed at 10⁰. The doctor stabilizes the ankle, while the calcaneus is inverted and internally rotated. The forefoot is then inverted. The doctor checks for any extra medial shift of the calcaneus.
The instability or feeling like the ankle joint might give way can also be reproduced by making the athlete stand on a single leg and do rotating motions of the leg and foot.
Doctors may want to assess the athlete during daily activities like walking, running, stepping down from a step, and hopping on the affected extremity. The activity levels of athletes with STS are assessed using the Ankle Disability Index.
Imaging
Athletes with subtalar joint instability and STS require diagnostic imaging. Radiographs of the subtalar joint are done with Broden's stress views. These are a series of oblique-lateral views. They are done ankle and foot inverted and supinated.
Stress fluoroscopy visualizes the motion of the subtalar joint. This occurs in real-time with low-level radiation. This is more advantageous than plain films as the doctor can use the movement to assess the instability from the STS.
MRI is the best method to visualize the structure within the sinus tarsi. It displays the interosseous and cervical ligaments. The most distinct finding for individuals is a bright signal in the sinus tarsi area which represents tissue with inflammatory cells and fibrosis. It also demonstrates alterations in the ligamentous structure of the interosseous and cervical ligaments and subtalar joint’s degeneration.
Lab Tests
Blood tests are not necessary to diagnose STS.
To learn how Sinus Tarsi Syndrome is treated Click Here
Physical Exam
During the physical examination, the doctor will always examine the un-injured ankle first. This might seem silly, but they need to know what the normal ankle looks like before any injury. They will examine the tibia, fibula, knee, and foot. The injured ankle is assessed for swelling, pain, deformity, ecchymosis, and any injury to the soft tissues. They will palpate the ankle and check any lacerations. Most doctors will start an examination from the tibia and fibula and then approach the ankle. They will check the nerve and blood supply to the joint. Sensations, pulses, capillary refill, and movement is assessed. They will test the passive and active range of motion and the ability to bear weight.
Imaging
Ottawa Ankle Rules state that X-rays for an are done only if there is a pain in either malleolus and one of the following:
Bone tenderness of the bone within 6 cm of either malleolus and inability to bear the weight that is about four steps, Ankle x-rays usually include 3 views. The AP view to assess soft tissue swelling. The Mortise view is taken with the foot in 15 degrees of internal rotation. It assesses the position of the talus. Finally, the lateral view which displays anterior and posterior avulsion fractures. It also shows ankle joint effusions if any. In some cases, plain films of the tibia and fibula are advised. A CT is done for posterior malleolus fractures.
MRI is not used in emergencies, but it can detect occult fractures and assess damage to the ligament and tendon. Ultrasound is an alternative to visualize fractures, ligament, and tendon injuries.
Lab Tests
Blood tests are not used to diagnose ankle fractures.
To learn how Ankle Fracture is treated Click Here
The physical exam starts with inspecting the ankle and foot for erythema or swelling, muscle strength, and testing of eversion and plantar flexion. The doctor will also check the peroneus longus tendon by resisting active eversion. The tendons are palpated during ROM of the ankle. As the fighter stands, varus and valgus alignment are examined.
To assess the stability of the ankle ligament, the ankle drawer test is done.
The fighter is asked to lay prone and the knee flexed to 90?flexion. The joint is examined for peroneal tendon subluxation.
Peroneal tendonitis develops pain and swelling gradually. The joint is therefore palpated for fluid and crepitation in the tendon sheath. Tendon subluxation is accompanied by painful clicking and popping at the lateral malleolus.
X-rays of the ankle is the main imaging modality for peroneal weakness. X-rays are done with weight-bearing and include AP, mortise, and lateral ankle views.
Additional X-ray views are the axillary or Harris heel view. The AP, lateral and oblique views of the foot are done to rule out other foot fractures. X-rays reveal avulsion from the base of the 5th metatarsal, avulsion fracture of the fibula, os peroneum, and retromalleolar groove flattening.
Ultrasound can evaluate the tendon in motion and identifying tears. MRI is to evaluate peroneus brevis tears. It can also visualize the surrounding tendons, edema, and bony deformities. CT scan evaluates bony deformity that might cause tendon dysfunction. It is also instrumental in guiding management.
Blood tests are not necessary for diagnosis.
To learn how Peroneal Tendon Weakness and Damage are treated Click Here
The physical examination includes a complete neurovascular examination. It also assesses strength and range of motion of the ankle. Any hindfoot pain worsened on plantar flexion is a positive plantar flexion test. If there is tenderness over the posteromedial ankle joint, then PAIS is suspected. The doctor will passively flex and extend the great toe. Any tenderness exhibited during the passive or active ROM, suggests injury to the FHL tendon.
Standard X-rays, CT, and MRI are used to PAIS. Generally, three views of plain X-rays are ordered: anteroposterior (AP), mortise, and lateral views. The lateral view is the best useful view to observe hindfoot pathologies like osteophytes, Stieda process, os trigonum, loose bodies, chondromatosis, and subtalar coalition.
Multi-slice helical CT evaluates osseous pathologies better. They provide more detail about the size, location, and several abnormalities in the bone. It assists the surgeon in pre-operative planning as well.
MRI assesses soft tissue lesions of the ankle. Usually, after a positive plantar test, Xray and MRI are ordered to view the structures of the hindfoot. An ultrasound diagnostic injection with a local anesthetic confirms the diagnosis.
No lab tests are required to diagnose PAIS. Radiology is diagnostic.
To learn how PAIS are treated Click Here
On physical exam, fighters with Achilles tendon rupture cannot stand. They cannot bear any weight on their toes. They have weak plantar flexion of the ankle. Doctors will palpate a tendon discontinuity. There will be signs of bruising around the ankle.
The Thompson Test is performed to assess for Achilles tendon. The doctor places the fighter in the prone position. The knee is flexed to about 90?. The foot and ankle are in the resting position. The doctor squeezes the calf. The degree of plantarflexion at the foot/ankle is noted. It is compared with the opposite side. A positive (abnormal) test indicates with pain Achilles rupture.
Plain films are done to rule out a fracture. Following the physical examination, the diagnosis is confirmed with an ultrasound or MRI.
Blood tests are not required to diagnose an Achilles tendon rupture.
To learn how Achilles Tendon Rupture are treated Click Here
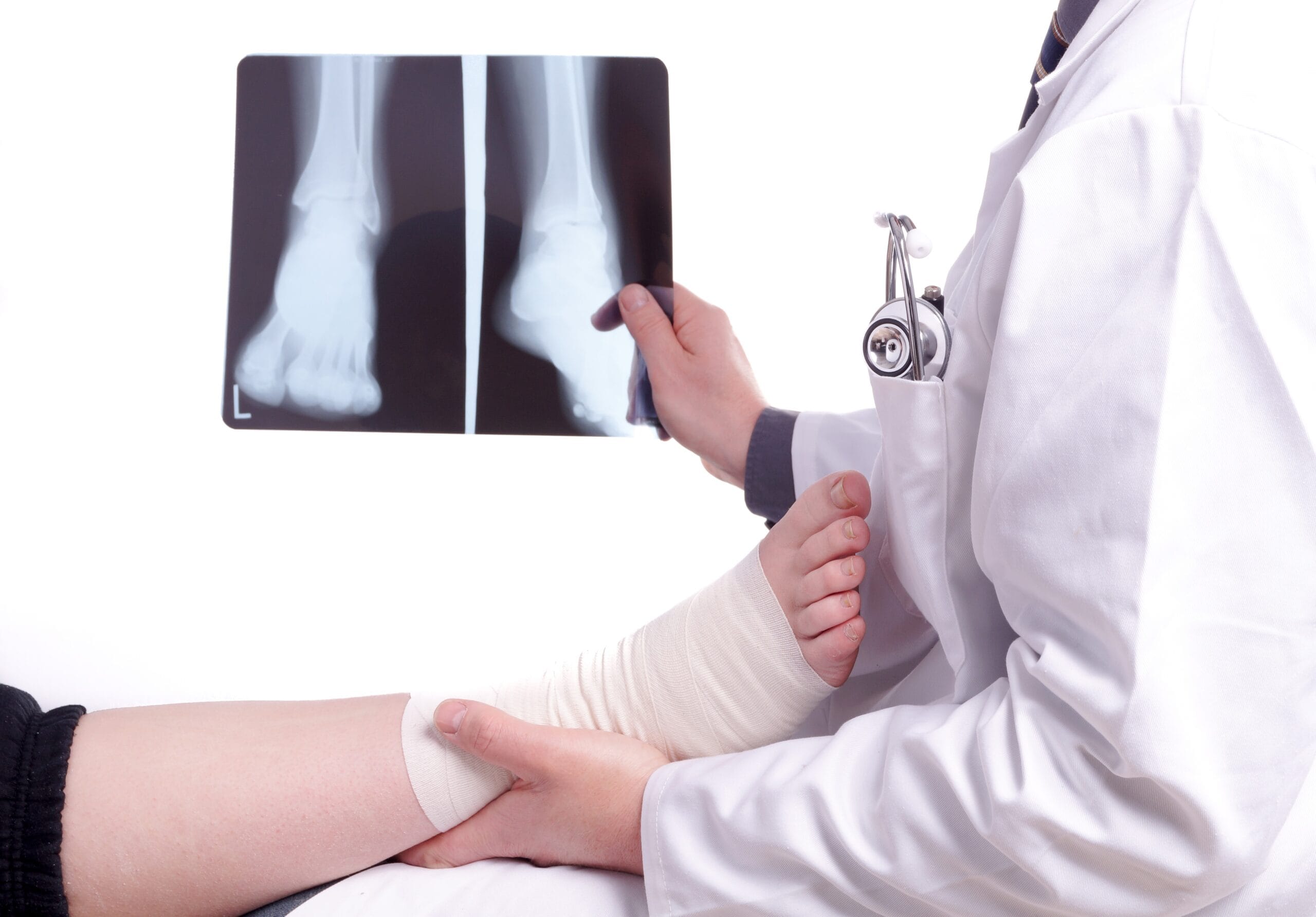
Common Diagnoses
Read our Common Diagnoses section to find out more about how various tests are used to diagnose injuries to the ankle joint.
Ankle Injury Treatment
The treatment of ankle injuries can include surgery, injections, medications, and physical therapy. The arsenal of treatment is vast and depends on the type of injury and its chronicity.
Injury Specific Treatment
Emergency Treatment
This is not a medical emergency. However, a long-term program of rehabilitation is advised for those with STS. It must include. Strengthening the muscles, taping, using braces, foot orthosis and balance, and proprioceptive training.
Medical Treatment
Athletes with STS have chronic inflammation. The resulting synovitis can be treated with a trial of nonsteroidal anti-inflammatory medication.
Cryotherapy, like an ice massage over the lateral ankle, can reduce inflammation and pain. Specific joint mobilization techniques are used in those subtalar joint pathology. Stretching the gastrocnemius, posterior tibialis, or peroneal muscles eases any muscle stiffness but they are introduced very carefully into the protocol.
Orthoses can stabilize the subtalar joint. Ankle braces are also helpful but they don’t stabilize the joint during a workout. Foot orthoses limit motion but reduce symptoms.
Footwear with a straight last, a firm heel counter, and rigid material through the midsole is advised in athletes with STS. The shoes are designed to support the foot and ankle throughout the training.
Taping or strapping limits the movements of the subtalar joint and the midfoot. The taping procedure combines a closed basket weave with a subtalar sling. This controls movements at the talocrural and subtalar joints. A modified Low-Dye tape using a calcaneal sling is an option. It supports the medial longitudinal arch of the foot It also controls pronation through the subtalar joint during ambulation. Taping is a precursor to shoes and foot orthotics.
Surgery is an alternative for those who fail rehab. An arthroscopic exploration and reconstruction of the subtalar joint are done. Arthroscopy allows precise examination of the subtalar joint and the sinus tarsi.
A synovectomy of the subtalar joint can be done. This is accompanied by an arthrotomy of the subtalar joint. It removes any fibrosis and chronic inflammation.
Surgical reconstructions of the ligaments are done by splitting the tendon and routing the graft through bone tunnels. The tunnels are made through the calcaneus and the talus.
Athletes with ligamentous reconstructions are immobilized for 6-weeks. After the surgery, a rehabilitation program is started. This is to restore mobility, strength, and balance in the ankle joint. Return to athletic activities starts 4 to 6 months after surgery.
Home Treatment
The hallmark of all treatment for STS is a training program to improve the stability of the subtalar joint. Joint stability depends on passive joint structures, muscular response, and neurological control. Since ligamentous tears lead to STS, the muscular responses and nerve control of the rearfoot needs to be reinforced. This is to compensate for the loss of passive structures.
These programs are multiphase processes. It starts at an appropriate level of activity and progresses higher levels as joint stability is maintained. Three phases are identified: Attain, Maintain, and Sustain.
The Attain phase determines postures or positions the athlete can do.
The Maintain phase develops coordinated isometric and eccentric muscle contractions of the muscles as they cross the joint. The Sustain phase integrates all of the necessary neuromuscular subsystems.
The Attain phase starts with the athlete standing. Single leg standing and the opposite limb at 30⁰ of hip flexion and 90⁰ of knee flexion with an eye open. Once the balance is achieved, it is done with closed eyes.
Maintain phase uses perturbation exercises. The star excursion balance test is one such activity. The athlete stands on a single leg and touches different lines that are drawn on the floor in a star pattern.
Standing heel raises, lowering exercises, exercises with a theraband, ball catching on a single leg are all exercises with pertubations for improving balance.
In the Sustain phase, the athlete learns to “close the chain.” He lunges and steps down from a 4-inch step into a single-leg standing. Once that is achieved, lateral lunge steps, lateral step downs, jumping, hopping in different directions can be added.
Running and accelerating, decelerating, forward and backward motions are slowly added.
Return to play depends on the fighter’s ability to move in all directions. It also depends on his ability to move at different speeds. Cutting and jumping maneuvers on firm surfaces requires days of recovery to prevent any stress on the joint.
Emergency Treatment
In the trauma bay, the fighter is assessed. ATLS guidelines are followed. After a primary survey and life-threatening injuries are ruled out, the ankle is examined. The nerves and blood supply are checked irrespective of the degree of deformity of the injured ankle. The skin is checked for skin tenting, this can delay healing. The goal of emergency treatment is to ensure there is blood flow to the ankle. After this, X-rays are obtained. Doctors will try and reduce the ankle fracture immediately and then splint the joint.
Medical Treatment
Pain management is done via NSAIDs, IV medications, hematoma block, or procedural sedation. After the fracture is reduced and splinted, the doctor will check the neurovascular status. The leg is kept elevated and another Xray is done. If the fracture is not reduced surgery is advised. Surgery includes Open Reduction Internal Fixation (ORIF) / or external fixation.
Stable fractures that are non-displaced can be treated conservatively. They are allowed to bear weight as tolerated. A walking boot is prescribed and an X-ray repeated in 1 week. If there is uncontrolled pain, numbness in the foot, tingling, increased swelling and change in their ability to bear weight, they are advised to seek medical care immediately.
Unstable fractures that are displaced, have talar shift, are bimalleolar, and trimalleolar will need surgery. Surgery is via open reduction internal fixation (ORIF). Instead, the joint can be cast for 6 weeks with non-weight-bearing status.
Home Treatment
Stable fractures that do not require surgery have an excellent prognosis. Gradually, they can bear weight and function normally at 6 to 8 weeks after injury. For fighters with unstable fractures that require surgery, full weight-bearing can occur at 12 to 16 weeks. However, it may take up to 2 years to function normally.
Conservative treatment is the first step. NSAID’s, ice, and immobilization are done initially. Physical therapy follows. Immobilization could be with a cast or controlled ankle motion boot. Using a lateral heel wedge, the shoes can be modified to unload the peroneal tendons.
If conservative therapy doesn’t help, then a steroid injection is an alternative. It is given around the peroneal tendon sheath. PRP (platelet-rich plasma) injections with ultrasound guidance improve tendinopathy. Conservative therapy is usually tried for 4 to 6 months to allow the resolution of inflammation.
Surgery is usually recommended for peroneal Tendonitis via open debridement and synovectomy or arthroscopic peroneal tendoscopy. Peroneal tendon subluxation is treated to restore the fibrocartilaginous rim, peroneal retinaculum, and periosteum to the fibula. The goal is to have the tendon glide smoothly.
If the superior peroneal retinaculum is torn, then open or endoscopic repair or reconstruction is necessary. Avulsion fracture of the fifth metatarsal or fibular groove should entail fixation or repair. Hindfoot varus alignment is corrected with hindfoot osteotomy.
Rerouting the peroneal tendons and bone block procedures are other alternatives. Peroneal tendon tears are treated based on the degree of the tear. Treatment also depends on whether the injury is acute or chronic. Debridement and tubularization are done when there’s partial tears of less than 50%. End to end repair is done where acute complete tears occur. Side-to-side anastomosis or Pulvertaft weave are done for chronic tears. Allograft reconstruction is another alternative for peroneal tears.
Following surgery, the outcomes are good. Most fighters can return to full activities within 13 months. Physical therapy and rehabilitation are essential following surgery and in conservative management.
Conservative treatment is the first step. This involves rest, no eliciting activity, physiotherapy, pain medication, and ultrasound-guided injections. Ultrasound-guided injections are a temporary fix.
Surgical management is advised for all those athletes who haven’t improved after 3 months of conservative treatment. Surgery is recommended early for professional athletes. Other alternatives include open treatment or arthroscopic intervention.
Arthroscopic procedures for PAIS are less invasive, have lesser complications, and shorter recovery time. For fighters with isolated PAIS, posterior hindfoot arthroscopy can be done.
Natural pain remedies such as INNER LINKS HERE arnica cream and/or dit da jow to reduce swelling, bruising and speed healing are effective, along with kinesio taping the ankle for additional support and pain relief. Other effective alternative healing methods include applying chopped onion and rosemary in a poultice as both have anti-inflammatory properties, massage, using a turmeric paste, essential oils, and various herbal supports.
Posterior impingement syndrome typically responds well to home treatment. R.I.C.E. therapy may be tried to ease pain, reduce swelling, and give the joint a chance to heal. Resting the joint is primary. Simple home treatments for chronic swelling include sleeping with the ankle and leg elevated on a pillow, and using an ace bandage or elastic ankle support when up and moving. Severe posterior impingement syndrome may linger and present problems with training, running, or simply getting to work because of pain, swelling, and/or weakness.
The primary difficulty here is if the injury is severe and not treated correctly, long-term problems may result. One reason for this is that a severe case of posterior impingement syndrome can be very difficult to identify and differentiate from a fracture or broken bone without taking an X-ray. Caution should be used, and medical help sought immediately if any of the symptoms below are present:
- 1The ankle is unable to bear weight
- 2Significant swelling occurs
- 3Deformity is seen in the joint
- 4Unable to walk more than four steps without significant pain
- 5Unable to move the injured joint
- 6Pain is felt directly over the bones of the joint
- 7Numbness is felt in or around the injured area
After surgery, a compression bandage is applied. They are allowed to bear weight as tolerated. They can also range their ankle. This is done as early as possible to prevent stiffness. Ankle immobilization is unnecessary. Only fighters with significant osseous injury need to exert more care. Others can stick to the above protocol and quickly return to the sport.
Immediately stop training, take the weight off leg, and seek medical advice from a professional as soon as possible. The initial treatment for Achilles tendon rupture is rest, elevation, pain management, with functional bracing.
These symptoms may point to other issues such as a ruptured Achilles tendon, which is why it is important to have this injury evaluated by a health professional to ensure proper treatment and healing. Conservative and surgical therapy are both alternatives. The rate of healing with serial casting or functional bracing is no different from surgery. In surgery, the tendon is surgically anastomosed. Return to fighting is delayed in surgery. Irrespective of therapy, all fighters, need physical and orthotic therapy. This will strengthen the muscles. It will also improve the ankle’s range of motion.
Rehabilitation is essential to regain maximal ankle function. There are several techniques for Achilles tendon repair. Every one of them reapproximates the torn ends. Occasionally, the repair is reinforced by other tendons such as the plantaris or the gastrocsoleus aponeurosis.
If a cast is used, it must be kept for at least 6-12 weeks.
For most fighters with Achilles tendon rupture, the prognosis is excellent. The majority can resume their previous activity without limitations. Continuous physical therapy can prevent its recurrence.

Common Treatments
Read more about how various therapies are used to treat ankle injuries in our Common Treatments section.
