Combat Arts Knee Injuries Overview
Jet Li began learning wushu at the age of eight in Beijing, China. It was intense. Jet Li described his wushu training as “bitter,” and as a teenager was forced to continue practicing eight hours a day for two days on a foot with the bone broken completely through. The knee joint is vulnerable, held in place by ligaments and tendons, and requires little pressure to damage. There are many types of knee injuries comprised mostly of sprains, strains, bursa or cartilage damage, or fractures.
Knee Injury Causes
Forceful martial arts kicks, both receiving and giving, jumping or landing incorrectly, pushing too far or fast during stretches can all easily cause knee joint damage. Most kicks in fighting and sparring hyperextend the knee and are considered poor form. In addition, weak quadriceps can lead to many different types of problems.
Coupled with hypertension of the knee, can lead to pain or discomfort around the knee and front of the thigh. Because of the mechanics of a kick, the knee is vulnerable to stress from long-term hyperextending of the knee, via the chamber – extension – chamber steps of the kick.
Knee Injury Symptoms
Symptoms of knee injuries include obviously deformed or displaced knee joints, inability to place weight on the leg, swelling or bruising around the knee, pain, limitations of movement, and stiffness.

Types of Knee Injuries
The injuries to the knee are plenty. Since the knee joint involves the femur, patella, tibia, fibula, tendons, and ligaments, this is a complex joint that is vulnerable to injury. These can include knee dislocations, fractures, contusions, tears, and sprains. In this section, let’s look at the common knee injuries seen in those in the combat arts. They include:
Meiscus tears, knee disolcations, ITBS, and ACL tears.
Strong Legs Muscles Are Crucial for Martial Arts Performance
Let Us Show You How to Get Stronger While Preventing Leg Injuries.
Related Injuries
A torn meniscus is a common problem in warrior and martial arts. The meniscus is the cartilage between the shinbone and thigh bone. A torn meniscus is one of the most common martial arts injuries because most kicks hyperextend the knee, which damages the meniscus. Not only is this damaging to the knee, but it’s also poor martial arts form.
UFC middleweight champion Michael Bisping severely tore his meniscus in 2017 and has had surgery to fix it and to further strengthen the weakened area. Bisping said they took fat from his stomach and injected it into his injured knee to help reinforce the problem area. He said this cutting-edge procedure will be “’ eliminating the need for some sit-ups 🙂 win, win!'”
There are two meniscus or menisci in each knee shaped like large wedges, and the outer one-third of it receives a good blood supply, while the inner two-thirds does not. The portion with a good blood supply typically heals quickly, but the part without it heals more slowly because it receives fewer nutrients.
Tearing the meniscus is exactly what it sounds like - a tear in the body of the cartilage. The majority of knee injuries in both martial arts and other sports activities are a torn meniscus.
Symptoms
A torn meniscus is usually very painful, which is a primary symptom. Other symptoms include:
Causes
The meniscus gets torn when powerful stressors place it in an incorrect position and then twist at the knee, like squatting incorrectly during a kung fu overhead throw or twisting a knee while grappling in jiu-jitsu. The meniscus tears when the knee is incorrectly rotated while weight is applied. In non-martial arts sports, the swift turns in basketball and soccer are prime examples. Other examples include:
To learn how Meniscus Tears is diagnosed Click Here
The kneecap or patella is an essential part of the knee that helps give strength and stops hyperextension of the leg. The kneecap normally sits in the patellofemoral groove. Injury from a kick or fall may cause it to dislocate from the patellofemoral groove.
Symptoms
A kneecap dislocation causes significant pain and deformity of the knee joint. A dislocated kneecap will result in obvious symptoms typically including:
Causes
A direct kick to the kneecap in krav maga, powerful fall onto the knee, or a hard pivot on a bent knee with a planted foot while doing an aikido overhead throw can dislocate the knee by knocking the patella out of the patellofemoral groove.
Martial artists who value the look of fancy kicks and moves may place undue stress upon their knees, thus causing dislocation and other injuries. Examples include:
To learn how Patella or Knee Cap Dislocation is diagnosed Click Here
Rothwell Keeps Fighting! Most people are going to react by falling to the ground in extreme pain. You don’t walk, much less fight on a torn ACL. Ben Rothwell blew his ACL trying to do a takedown on Gilbert Yvel. Then Rothwell kept fighting another three full rounds on a blown ACL—and still won--by unanimous decision.
The Anterior Cruciate Ligament (ACL) injury is a common knee injury mostly found in high impact and endurance sports. The ACL is one of four ligaments within the knee that connects the femur to the tibia. It prevents the tibia from sliding forward in front of the femur and provides rotational stability to the knee. An ACL injury occurs because of powerful pressure placed upon the knee joint, femur, tibia, and/or patella.
Most people have seen a sporting event where a player needs to be carried off the field or mat after falling and clutching their leg in agony. Symptoms include a loud "popping" noise or sensation at the time of injury, knee no longer supports weight, intense pain, and swelling. When an ACL tear or other damage to the knee has occurred, it will be immediately noticeable because of pain or difficulty in continuing with training. Major symptoms include:
ACL injuries occur due to extreme stress on the lower leg and/or rotation stress. Generally, rotational stress or force against the back of the leg causes damage. ACL injuries occur when the martial artist does a judo high double flying kick and lands incorrectly, executes sudden stops, quick directional changes at high speed, receives a direct blow to the knee, or intense jumping then landing wrong. ACL injuries most commonly occur during sports that involve kicking, fast weight shifts, pivots, quick stops, jumping, or directional shifts. Examples include:
To learn how Acl Injury are diagnosed Click Here
Iliotibial Band Syndrome or ITBS is a very common sports injury. Iliotibial band syndrome occurs from the intensive overuse of these muscles. It is one of the leading causes of lateral knee pain in runners and bicyclists, occurring so often in long-distance runners that it is considered a “runner’s injury.”
The iliotibial band is a strong, thick length of fibrous tissue that begins above the outside of the hip joint at the iliac crest in the pelvis, crossing both the hip and knee joints, and extending down the outside of the leg to the shin bone or tibia, inserting just below the knee. The IT band is one of the hip abductor muscles responsible for the movement of the hip away from the midline.
This band is a crucial part of the stabilizing structure of the outside of the knee and works in conjunction with other muscles to bend and straighten the knee. This band of tissue is essential to knee stabilization while running, giving stability and support to the outside of the knee joint. It works in conjunction with thigh muscles to strengthen the knee joint and keep it in place.
This overuse injury causes pain on the outer part of the knee, often when the heel hits the ground during running. The IT band is continually rubbing and moving across the femoral epicondyle as the knee flexes and extends. Also, where the iliotibial band crosses, between bone and muscle is a pillow-like protective bursa which helps ‘oil’ motion and smooth movement of the band.
The inflamed iliotibial band will not slide smoothly as it should across the femur, and instead creates pain. During certain movements such as running, bicycling, and jumping, this repeated flexing and extending of the knee causes the IT band of connective tissues to become inflamed.
When this overuse injury causes pain and tenderness, most often just above or below the knee joint, it means inflammation has formed in the iliotibial band. Pain is typically caused by compression from abnormal movement patterns of the femur. Iliotibial band inflammation also often occurs in athletes who repeatedly squat, which includes runners and weight-lifters. It is apparently due to weakness in the hip and butt muscles, lack of flexibility in the muscle, and mechanical imbalances in the body such as incorrect body mechanics involved in leg movements, step landing, or weakness in the lower back, hips, pelvis and/or knees.
There have been many theories about what causes ITBS, but up until recently the mechanisms for it occurring have been very poorly understood. The gluteus maximus and gluteus medius are major muscles in the butt that are used to control and position the pelvis, and also stabilize the leg when kicking, running, or bicycling. When the pelvis moves incorrectly, the IT band is placed into an incorrect position, as well, putting it at risk for injury.
Bicyclists and runners especially often do not engage in strength training. Martial artists often overdevelop one side of the body to the detriment of the other or focus more on the upper body than lower. Martial artists who suddenly seek to up their game, increasing hours spent training, running, and weight lifting will often develop iliotibial band syndrome. These omissions and/or sudden increases without correctly balancing the strength of critical muscle groups are crucial to understanding why fighters and endurance athletes may develop ITBS.
Primary causes for developing IT band syndrome include:
To learn how IT Band Syndrome are diagnosed Click Here

Common Injuries
Learn more about common knee injuries like sprains, contusions, and dislocations in our Common Injuries section.
Knee Injury Diagnosis
To diagnose injuries in the knee joint, doctors usually rely on several tests and maneuvers during the physical exam. This is to isolate which ligament, muscle, or tendon is involved in the injury. For loose bodies or bone injuries, imaging is used.
Injury Specific Diagnosis
Physical Exam
The physical examination of the knee joint starts with the inspection of the knee for edema. Doctors will palpate the joint line and range of motion (ROM) while standing and lying down. They will test the muscle strength test. They will check for anteromedial and anterolateral joint line tenderness. This is a special test. It is done with the knee at the edge of the table. The knee is flexed at 90⁰. This is specific to meniscus tears. Additionally, flexion or extension ROM is affected in different types of tears and how much fluid effusion is present in the joint needs to be seen.
Most fighters will have an antalgic gait if observed. This is a gait to avoid pain, the stance phase is shortened compared to the swing phase. The doctors will also observe if there is increased pain on single or double-leg squatting.
Provocative tests are done to detect meniscal tears. One such test is the Thessaly test. Here the fighter stands on one leg. The examiner helps him balance. The fighter squats down to 20⁰ of flexion and internally or externally rotates the knee. This motion is continued through active adduction and abduction of the hip.
Another test is McMurray's test. It involves passively extending the fighters’ knee as he lies down. The knee goes from a fully flexed position to 90⁰ flexion. This motion is continued through full external or internal rotation.
Apley's compression test is another diagnostic test. Here the fighter lies prone. The knee is passively flexed to 90⁰. Following flexion, it is externally or internally rotated. This provides the axial compressive force.
In all of these tests, any reproducible pain in the knee during the exam is indicative of a meniscus tear.
Imaging
X-rays must include AP, lateral, oblique, sunrise, and weight-bearing views. This is to assess fractures of other bones. The best test for this is an MRI. It can be done using arthroscopy. MRI can diagnose and characterize meniscal tears.
Lab Tests
Blood tests are not needed to diagnose a tear in the meniscus. Radiology usually suffices following the physical exam.
To learn how Meniscus Tears is treated Click Here
Physical Exam
On physical examination, the knee joint has typical findings when it is an acute dislocation. There is a joint effusion or hemarthrosis. The knee is swollen and has fluid or blood within the joint space. This is not so in a chronic dislocation. Joint dislocations also demonstrate alignment abnormalities. These include tibial torsion, femoral anteversion, patella alta, genu recurvatum, genu valgum or varum, pes planus. The ligaments of the knee appear to be lax.
The doctor will palpate the knee and surrounding structures. They will check for tenderness or irregularities along with the patella. They inspect and palpate each pole of the patella, superior, inferior, medial, and lateral. The range of motion through flexion and extension is checked. The doctors look for crepitus or restrictions in mobility. Following this, they will examine the collateral and cruciate ligaments.
Some fighters with a dislocated patella exhibit a positive J sign. This is a sign where there is excessive lateral patellar deviation while the knee goes from flexion to extension. The normal patella can be moved medially and laterally between 25% and 50% the width. In recurrent dislocations, the patella glides even further.
Fighters with patella dislocations may have a positive apprehension test. In this test, the knee is relaxed in 20 - 30⁰ of flexion. Then the patella is moved laterally. The test is positive if the fighter guards against this motion or hesitates with pain.
Imaging
Plain Radiographs with anteroposterior (AP) and lateral radiographs of the affected knee are necessary. Patellar or sunrise views are also very helpful. They identify fractures, loose bodies, and any misalignment.
Anatomic risk factors like patella alta are identified on plain films. Disruption of the Blumensaat line can also be seen.
Lateral views can assess trochlear dysplasia. The 'crossing sign' and the 'double contour sign' is present if the fighter has a convex trochlear groove or underdeveloped medial condyle that contributes to the dislocation.
The Merchant or sunrise view assesses the patellar tilt. It is an axial view taken at 45 degrees of flexion.
CT scan measures the TT-TG (Tibial tuberosity-Trochlear groove) distance. This is important for the management of patellar dislocation. The CT scan identifies osteochondral fractures if any and aids planning for surgical intervention.
Magnetic resonance imaging looks at the soft tissue of the knee joint. If complete dislocation has occurred, a characteristic bruising pattern of the femoral condyle and medial patella is seen. Disruptions of the MPFL (medial femoral epicondyle insertion) is observed. MRI can diagnose articular cartilage damage and osteochondral lesions. It can display trochlear anatomy if there is trochlear dysplasia.
Lab Tests
No blood tests are needed to diagnose patella dislocation. Radiology is diagnostic.
To learn how Patella or Knee Cap Dislocation is treated Click Here
The physical exam will include assessing joint stability, mobility, and strength. Doctors will palpate and evaluate associated injuries.
Multiple maneuvers are used to specifically test the ACL. This includes the anterior drawer, the pivot shift, and the Lachman tests.
The anterior drawer test is done with the fighter lying supine. His affected knee is flexed to 90⁰ and the foot is in a planted position. Don’t be surprised if a doctor sits on the foot to plant it firmly. They will then hold the proximal tibia with both hands and pull anteriorly. Any excessive anterior motion and instability are confirmatory for an ACL tear. The contralateral knee is also tested to check that the fighter doesn’t have any increased ligament laity. This test is very specific for chronic tears of the ACL.
The pivot shift test is also done with the fighter lying supine. The doctor will hold the fighters’ lower leg. The knee is usually extended and the hip flexed to about 20 to 30⁰. He will internally rotate the tibia with one hand and place valgus stress on the knee with the other hand. In this position, the knee is flexed. This causes stress, instability, and causes the subluxation of the ACL of the affected knee. As the knee flexes of the tibia is subluxated posteriorly any “clunk” indicates a positive test. This test is difficult for fighters who have guarding but it is very specific and diagnostic.
The Lachman test is done with the fighter lying in the supine. The knee is flexed to about 30⁰. The doctor stabilizes the distal femur with one hand. If there is an anterior translation with a mushy soft end feeling, it is a positive test. The doctors will compare the movement with the opposite side. They will check associated injuries to the medial or lateral collateral ligament, posterior collateral ligament, or meniscus.
ACL injuries are diagnosed clinically but they are confirmed with imaging by magnetic resonance (MRI). MRI is the main modality to diagnose ACL pathology. Arthroscopy can also diagnose and differentiate complete from partial tears, and acute from chronic tears. Arthrography can also be used however this is rare as it is invasive and requires anesthesia.
On MRI, ACL tears demonstrate primary and secondary signs. Primary signs include edema, discontinuity of the fibers, and alteration of Blumensaat’s line. They are usually seen in the midportion of the ligament. Secondary signs include bone marrow edema, a second fracture, an associated medial collateral ligament injury, or anterior tibial translation of greater than 7 mm.
Radiographs rule out fractures and osseous injuries. Generally, they are not necessary for diagnosis. On radiographs, you can see features like a second fracture. A second fracture is an avulsion fracture at the site iliotibial band insertion. X-rays may also reveal arcuate fractures. These are avulsion fractures at the proximal fibula. They take place at the lateral collateral ligament or the biceps femoris tendon. Plain films can show joint effusion and the deep lateral sulcus sign. This is a notch on the lateral femoral condyle. It has a depth of more than 1.5 mm.
CT is not used to evaluate the ACL. It can accurately detect an intact ACL.
Blood tests are not required to diagnose an ACL injury.
To learn how Acl Injury are treated Click Here
The first step is the physical examination of the knee. Any knee misalignments such as genu varum, genu valgum, recurvatum, and procurvatum are noted and examined. The doctor will check for laxity and knee effusions. Palpating the knee is painful and the doctor will need to examine for any crepitus with a range of motion tests.
Special tests for ITBS include the Noble and Ober tests.
In the Noble test, the physician palpates the lateral femoral epicondyle. He then extends the knee from 90⁰ of flexion to 0⁰ of extension. If there is any pain at 30⁰ of flexion, it is a positive test.
In the Ober test, the fighters lie down in the lateral recumbent position. He flexes the knees to 90⁰. The doctor stands behind him. He then abducts and extends the affected hip and supports the knee. Any restriction and pain to the lateral knee is a positive test.
An MRI may be recommended to search for inflammation on or around the iliotibial band, and to check for other possible causes of outer knee pain such as torn cartilage or meniscus tear, muscle, ligament or tendon inflammation or tear, kneecap, and femur pain. Typically, diagnosis is made with an examination, and X-rays and MRI images are not needed.
Blood tests are not necessary to diagnose ITBS.
To learn how IT Band Syndrome are treated Click Here
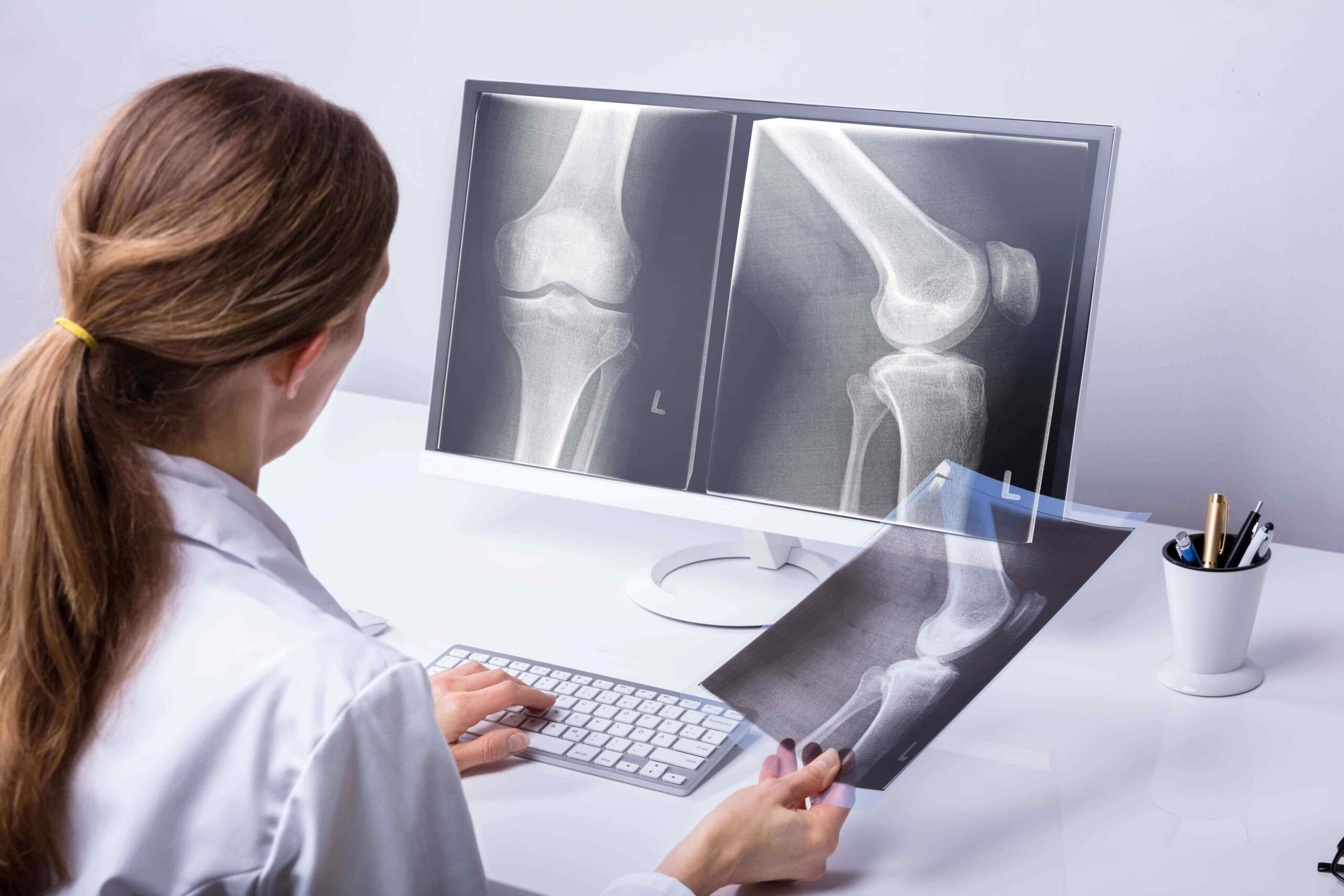
Common Diagnoses
Learn more about how physicians assess injuries through visual inspection, lab tests, x-rays, and other methods in our Common Diagnoses section.
Knee Injury Treatment
Knee injuries are treated in several ways. For mild injuries, RICE therapy is adequate. However, since the knee is a complex joint, injury is multifocal and hence a variety of therapies are required. Complex and chronic injuries may require surgical intervention.
Injury Specific Treatment
Emergency
The initial treatment of a painful knee suspicious of a meniscal is conservative. RICE principles and pain control for, the cornerstone of the treatment protocol. To protect and compress the knee, a brace or knee sleeve is helpful. Do not limit joint movement. Start knee and ankle exercises at the earliest. This will help the joint heal fast and clear any edema within the joint.
Medical
Treatment depends on severity. Home healing methods may be used if the injury is mild. Physical therapy may be required to strengthen muscles and tendons. Surgery may be required in extreme cases. Studies of medical literature have discovered that the failure rate for meniscus surgery ranges as high as 45% overall.
Surgical treatments available include:
Stem cell treatment uses the body's stem cells to help repair damaged tissues. This treatment works well for a torn Meniscus.
Home Treatment
Physical therapy is very important for the treatment of the tears of the meniscus. This is irrespective of treatment, medical or surgical. During the first 6 weeks, knee flexion ROM and the weight-bearing exercises are restricted. Most fighters return to plan with full mobility of the knee after a prolonged rehabilitation program.
Emergency Treatment
Stop training or fight events, commence emergency treatment. Immediately immobilize the knee with splints made of cardboard, wood, dowels, magazines, etc., and take an injured fighter to hospital, or call 911 for help. If the fighter has dislocated his knee for the first time and there are no loose bodies, initial treatment is conservative. This includes pain management with analgesics and ice to reduce pain and swelling. Physiotherapy is started and activities are modified until the injury is healed.
Medical Treatment
In acute dislocations, doctors will try to promptly reduce them. This is done in the emergency department with sedation as needed. It involves flexing the hip, while simultaneously applying gentle pressure to the lateral patella. The pressure is applied in a medially while extending the knee slowly. Occasionally, doctors may do this with the fighter sits with legs hanging off the side of the bed.
The doctors may use a brace like a J brace or a patella stabilizing sleeve. This allows the soft tissues to heal over 2 to 4 weeks. After the removal of the brace, physiotherapy should be started. Any physiotherapy must focus on strengthening the quadriceps and vastus medialis oblique. The rehab program also concentrates on strengthening the core and proprioception. Weight-bearing is permitted as much as the fighter can tolerate.
Arthroscopy is done to treat an osteochondral fracture, with open repair of the fragment. Surgery is warranted if the fighter has a dislocation for the first with a loose body. If MRI shows disruption of MPFL, the patella is subluxated or recurrent dislocations occur then surgery is preferred. Also, for those fighters in whom medical management fails or those with risk factors for multiple dislocations, surgery is advised.
Proximal and distal realignment is done via many surgical options. This includes arthroscopy with or without open debridement, MPFL repair or re-attachment or reconstruction, or lateral release.
Fulkerson osteotomy can be done. Here, the anterior tibia is cut at a certain angle. This allows the cut fragment to move anteriorly and medially. If there is a rotational deformity, a derotational osteotomy of the femur is done.
Trochleoplasty is only done in fighters who have recurrent dislocations with a convex or flat trochlea. It’s only done in severe cases.
Home Treatment
Postoperative rehabilitation depends on the type of surgery. Recovery from a lateral release is the shortest. Recovery time from surgery can take anywhere from 6 months to a year.
After surgery, physiotherapy is necessary after initial immobilization. Fighters are not permitted to return too early to contact sports. They must have significant physiotherapy to strengthen the surrounding muscles and the core. Fighters can wear slip-on knee braces during early recovery.
Acute injuries require “RICE” therapy. This means rest, ice, compression of the injured knee, and elevation of the extremity. Fighters are not permitted to bear weight. They can use crutches or a wheelchair. Pain management is with NSAID’s. ACL injuries are treated surgically or medical depending on the type of injury and its severity.
The martial artist who experiences a full tear may require surgery since a torn ACL will not heal by itself. It must be reattached but cannot simply be sutured or stitched back together. ACL surgery to repair a torn ligament requires a tissue graft from hamstring tendons, patellar or quadriceps tendon. The ACL ligament is then reconstructed to restore knee strength and stability. It may take 6 months or more for the ACL and joint to return to their former strength and power. Operative treatment is typically done with a tissue graft.
Resting the injured area, staying off the joint, adding an ace bandage, or using a brace may be enough to allow recovery of minor tears, although rehabilitation and physical therapy exercises are usually required. Physical therapy exercises and rehab will strengthen the supporting muscles and help to ensure the joint is not injured again because of lingering weakness.
ITBS is not a medical emergency. The first step in treating it is conservative nonoperative management. The fighter must refrain from any inciting activity until there is no pain. Intermittent cryotherapy can treat acute flares. A gradual return to play is recommended once there’s no pain while moving or palpation by a doctor. Physical therapy is essential and must focus on the stretching of the ITB. Exercises to strengthen the abductors are also good to lengthen the ITB and reduce any tension.
Manual therapy such as myofascial release is also helpful. It is done with a foam roller and breaks up adhesions.
NSAID’s are prescribed to reduce inflammation and pain. Corticosteroid injections also provide similar relief. To prevent their recurrence, athletes are advised to modify their shoes and wear foot orthosis or braces. Most fighters can return to activity within 6 to 8 weeks with medical treatment alone.
The progression of activity has to be gradual. It must start with a week of running on a flat surface every alternate day. Avoid any downhill activity. After 4 weeks of brisk runs, the distance and frequency are increased. If there is no pain at this point, a slope can be added to the surface.
Surgical intervention is recommended for those athletes where medical management has failed even after 6 months of treatment. Surgery is done via percutaneous or open ITB release. The ITB lengthening with a Z-plasty, open ITB bursectomy, and arthroscopic ITB debridement are other options. In some cases, doctors might resect a triangular portion of the ITB band over the lateral femoral epicondyle.
ITB bursectomy is another option where the ITB bursa is removed completely leaving the ITB intact. Minimally invasive techniques where the lateral synovial recess is resected have also been done.
Fast-paced running on flat surfaces limit the time in the so-called "impingement zone.” Therefore, it is encouraged. Those in the combat arts must change their shoes regularly to prevent uneven wear of the soles as they train. Physical therapy is very important. Exercises to strengthen the abductors and loosen the ITB tension form the cornerstone of physical therapy in ITBS.
Common Treatments
Learn more about how healthcare professionals treat injuries using physical therapy, medications, surgery, and other approaches in our Common Treatments section.
