Combat Arts Toe Injuries Overview
The toes are particularly prone to injury because of their many small bones and primary position in movement propulsion and supporting the body’s weight. Toe injuries may include contusions or bone bruises, stress fractures or broken bones, sprain, strain, pinched nerve, or tendonitis.
Toe Injury Causes
Toe injuries may occur while incorrectly kicking the heavy bag, toes connecting with opponent’s elbow or knee during a kick block, toes hitting a hard object such as a rock while running, jumping, or landing wrong after an overhead throw.
The reasons for toe pain are extremely varied and range from stubbing a toe on the mat, inflammation or pain from kicking a bag or opponent incorrectly, extreme jumping or kicking, muscle weakness, pinched nerve, bursitis or bunions, tendonitis, fractured or broken bones, improper gait and mechanical movement issues, too much time spent on the feet or badly fitting shoes.
Toe Injury Symptoms
Typical toe injury symptoms include:

Types of Toe Injuries
The toes or metatarsals are vulnerable to acute injury and chronic injury. Two specific injuries that are addressed are common in martial arts. The first is toe fractures and the second condition is turf toe.
Related Injuries
Overview
Olympic Judo silver medalist Travis Stevens sustained a broken toe during an injury to Mexico. He calls the injury small but frequent in martial arts. In grappling and many other combat sports, injuries to the toes are considered common. Yet, we don’t recommend his method of treating or dealing with toe injuries. We also don’t recommend that a combat artist should self-treat unless the injury has been confirmed.
Symptoms
Causes
One of the most common toes to fracture is the 5th metatarsal. However, any of the metatarsals are vulnerable to injury during rapid, violent, and forceful movements. Commonly, the metatarsal shaft, the proximal fifth metatarsal, and the proximal first through fourth metatarsals are always injured and they have specific tests and treatment plans based on whether the injury is acute or chronic.
To learn how Toe fractures is diagnosed Click Here
Overview
Turf toe occurs due to forceful hyperextension of the first MTP joint. It was first commonly described in players who played on turf like soccer. However, ironically, it has been observed in martial artists and athletes who play on artificial mats and turfs. The reason being these surfaces are far more rigid.
Symptoms
Causes
The first MTP functions as a hinge and a sliding joint. There is little bony stability between the convex metatarsal head and the concave base of the proximal phalanx. A series of attachments via the capsule, ligaments, and musculotendinous structures support the complex joint.
The strongest stabilizer of the first MTP joint is the plantar plate. It is made of the thickened joint capsule. Any violent motion, sudden kick, toe getting stuck against the mat can disrupt the attachment to the transverse head of the adductor hallucis, the flexor tendon sheath, and the deep transverse intermetatarsal ligament. The injury is classified based on the degree of injury to the plantar plate:
To learn how Turf Toe is diagnosed Click Here
Overview
Any direct blow or a crush injury to the distal toe can damage the nail bed. As blood enters the space it exerts more pressure. Nailbed avulsions can be associated with subungual hematomas, fractures of the finger, or avulsion of the finger joint. In martial arts, nail injuries take place due to sudden moves.
Symptoms
Causes
Sometimes, simply a toe into an opponent’s gi can cause a nailbed to get avulsed if they jerk away or the movement is sudden and forceful. A crush injury where the toe is crushed under an opponent or a finger fracture due to a fall can also cause a nail bed injury.
To learn how Nailbed injuries are diagnosed Click Here
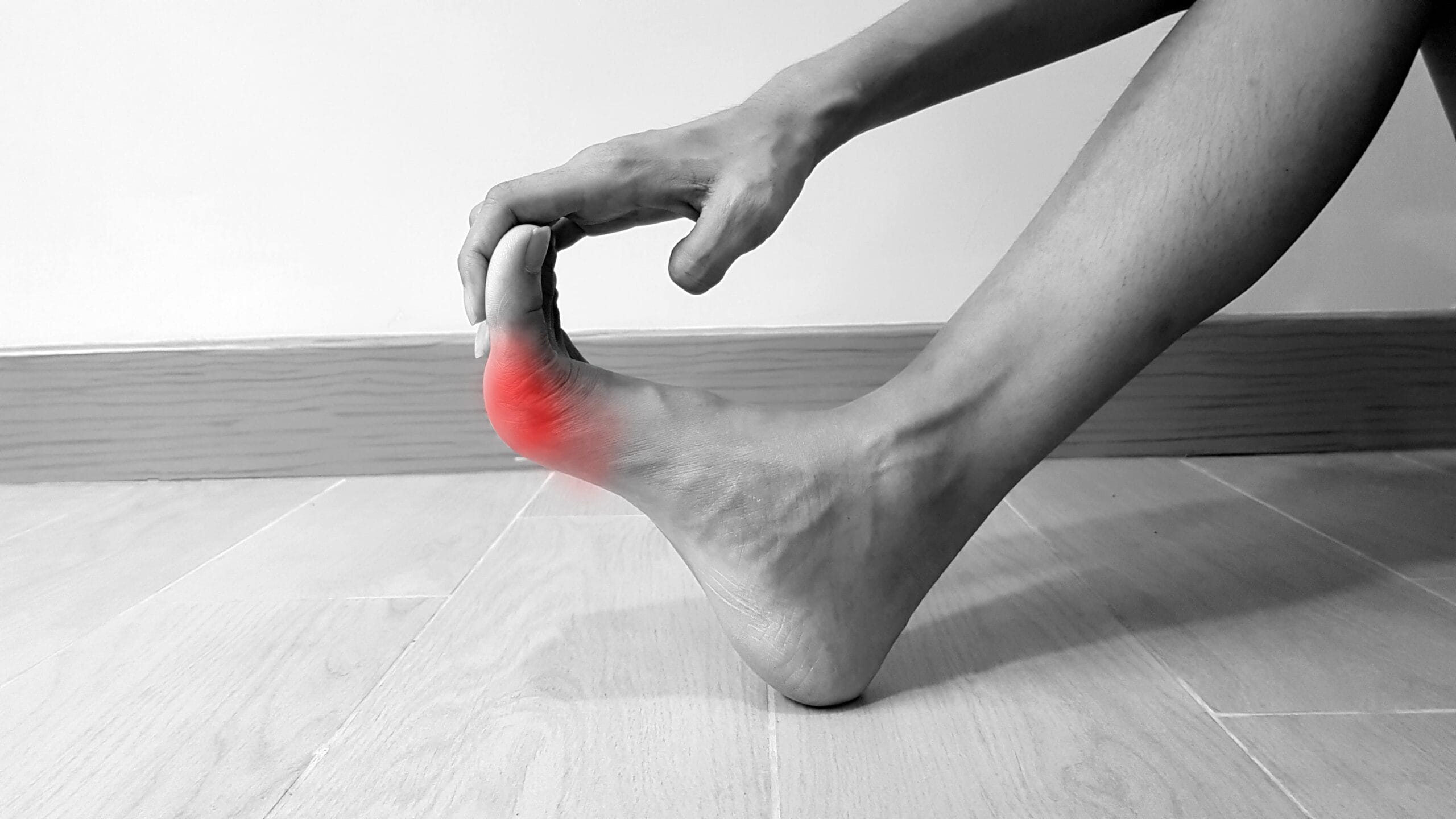
Common Injuries
Our Common Injuries section has more information on dislocations, sprains, and strains of the toe.
Toe Injury Diagnosis
Toe injuries require imaging to confirm any damage to the small bones and the ligaments that hold the bones together. They confirm preliminary findings made via physical exam. Blood tests are not required unless gout or other arthritic conditions are suspected.
Injury Specific Diagnosis
Physical Exam
During the physical exam, the skin is examined to check for any open injuries. These may require debridement and changes the treatment plan. Doctors will palpate the foot for tenderness, swelling, and ecchymosis. They will test the range of motion of the foot and toes. Some martial artists with toe fractures find it difficult to evert the foot or have pain with resisted foot eversion.
Imaging
Plain films are done to evaluate foot fractures. The views usually include AP, lateral, and oblique images. The fractures especially of the 5th MTP are divided into zones.
In zone 1 injuries, the fracture line is closer to the 4th/5th intermetatarsal joint.
In zone 2 injuries, the fracture line extends into the 4th/5th intermetatarsal joint.
In zone 3 injuries, the fracture line is beyond the 4th/5th intermetatarsal joint.
Based on plain film imaging, the stress fractures in the 5th MTP are categorized by the Torg classification system:
Type I fractures: that are early, with no sclerosis and minimal periosteal reaction.
Type II fractures: that are delayed, with sclerosis, and periosteal reaction.
Type III fractures: where there is non-union, and the medullary canal obliterated by sclerosis
CT and MRI are used if the bone is not healing or if there is a stress fracture that’s not seen on a plain film.
Lab Tests
Blood tests are not usually required unless gout or other arthritis is suspected. If these conditions exist, doctors may order Rh factor, CRP, Uric acid, and other blood tests.
To learn how Toe fractures is treated Click Here
Physical Exam
During the physical exam, the foot is inspected and palpated. The ROM, muscle strength is tested along with special testing.
The doctor will first inspect the toe for swelling and ecchymosis. They will evaluate the gait pattern and note if an antalgic gait is present that favors toe-off. During the exam, in a fighter with turf toe, toe raises on the affected side are extremely difficult to perform. Doctors will also look for deformities of the joint including dislocation, hallux valgus, or hallux varus.
While palpating, they will look for point tenderness over the plantar aspect of the MTP. Doctors will check for tenderness over the medial and lateral, and dorsal joints.
Both active and passive ROM tests are done. On passive ROM, the martial artists complain of pain on extension of the MTP. On active ROM, flexion will cause pain in the MTP.
Muscle strength is tested by making the martial artist flex their toes or extend toes against resistance. Abduction can also be done to test muscle strength.
Some special tests for turf toes include performing a valgus and varus stress test of the first MTP joint. This is to check the stability medially and laterally. The vertical Lachman test examines the degree of vertical translation. The test is positive when the MTP has more laxity than the opposite side.
Imaging
The plain films should include these views; AP, lateral, and axial sesamoid weight-bearing. Any fracture or dislocation can be seen on a radiograph. Generally, bilateral radiographs are taken. This is to compare the migration of sesamoid bone.
MRI without contrast is done to visualize soft tissues. The MRI can see a plantar plate or any injury in the surrounding soft tissues. MRI can detect inflammatory and degenerative changes in the joint.
Based on the physical exam and the imaging, turf toe is graded. The Anderson classification system grades it on a scale of 1-3 as follows:
Grade 1: Acute sprain, no bone fracture, no joint instability, normal ROM, can bear weight.
Grade 2: Partial tear of the capsule or plantar plate, painful ROM, swelling, painful weight-bearing.
Grade 3: Complete tear of the plantar plate or capsule, migration of sesamoid bone, tenderness, decreased ROM, swelling, inability to bear weight.
Lab Tests
Blood tests are not required to confirm the diagnosis of turf toe. The physical exam and imaging are more than enough to make a diagnosis.
To learn how Turf Toe is treated Click Here
Physical Injury
The physical examination of the nailbed is done where there is appropriate lighting to visualize the injury carefully. An assessment can be made based on the history but a physical exam may reveal hematomas or hidden fractures. The doctors look for lacerations, closed or open fractures, and any associated amputations of the toe-tip.
Imaging
Evaluation will include assessing the toe. The associated toe is examined for sensation, the range of motion at the interphalangeal joints, and capillary refill. If injuries to the bones, joints or soft tissue is suspected in addition to the nailbed, then X-rays of the affected toe and foot with two or three views are done.
Lab Tests
No lab tests are required to diagnose injuries to the nailbed.
To learn how Nailbed Injuries are treated Click Here
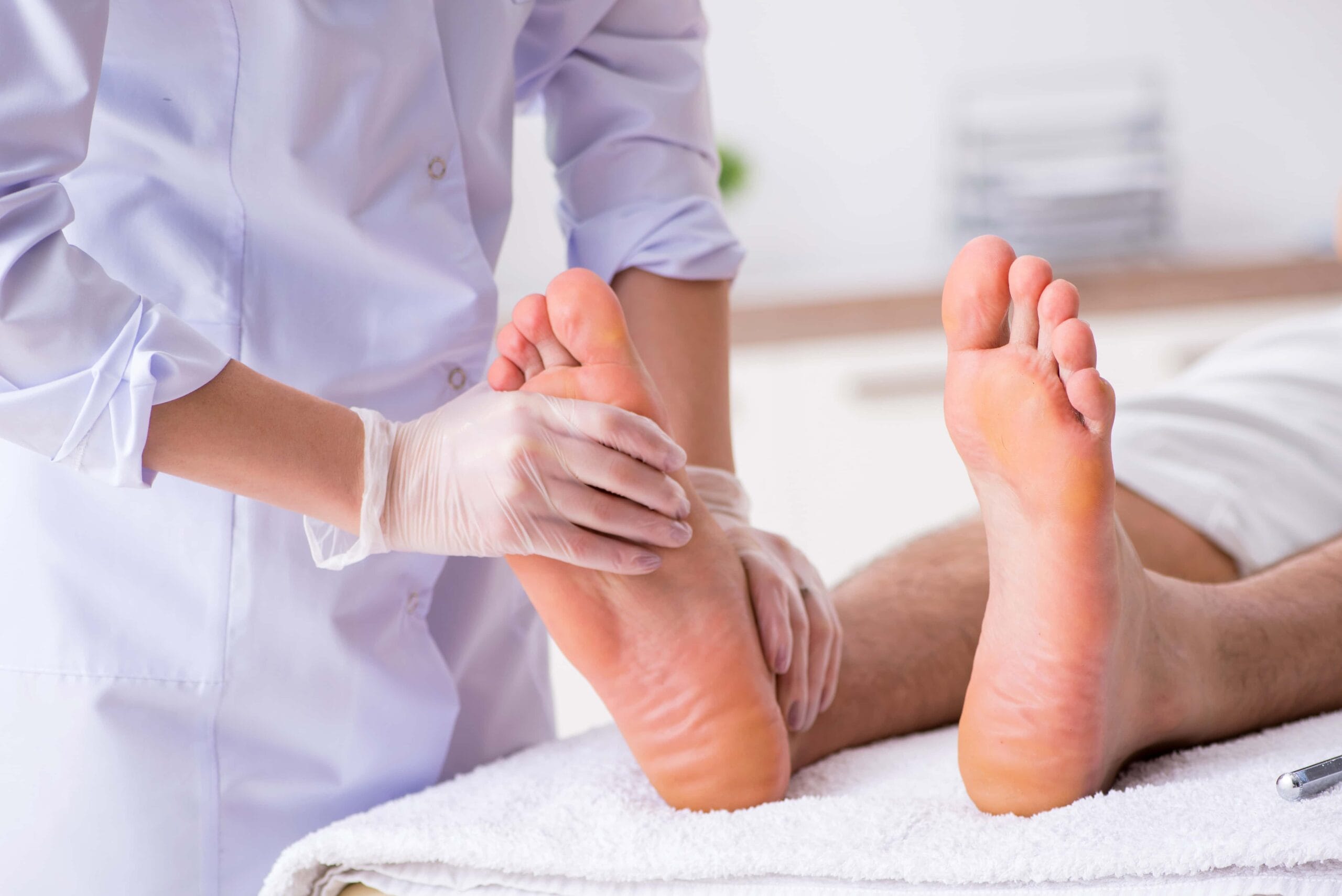
Common Diagnoses
Read through our Common Diagnoses section to find out more about how injuries to the toes are diagnosed.
Toe Injury Treatment
The treatment for toe injuries is based on the type of injury. Pain management and physical therapy are integral to the therapy.
Injury Specific Treatment
Emergency
For all the martial artists diagnosed with nondisplaced zone 1 injuries, conservative treatment is started. This includes walking boots, hard-soled shoes, walking casts with protected weight. Once the pain eases after 3-6 weeks, weight-bearing is allowed as tolerated. If the fracture involves more than 30% of the articular surface or the step-off is more than 2mm then surgery is advised. This can include ORIF, closed reduction, and percutaneous pinning, or excision of the fragment.
Medical
Martial artists with nondisplaced zone 2 injuries or Jones fractures are also treated conservatively. They are given a short leg cast with no weight-bearing for 6-8 weeks. As the plain films show healing of the bone, weight-bearing may be permitted.
In competitive athletes, surgical therapy is preferred. Displaced fractures are also surgically treated. The surgical techniques include intramedullary screw fixation, tension band constructs, low profile plates, and screws.
Diaphyseal zone 3 stress fractures are more complicated to treat. So an initial trial with a short leg cast and no weight-bearing is the first step. In some cases, immobilization for about 20 weeks is necessary to prevent non-union. Competitive athletes or those with Torg Type II or III fractures may require surgery. These include intramedullary screw fixation with or without bone grafting.
During, bone grafting, a 0.7 by 2.0 cm rectangular section of bone is removed at the site of the fracture. It is replaced by an autogenous corticocancellous bone graft. This graft is usually taken from the distal tibia. The sclerotic bone is removed before the graft is inserted.
Other fractures of the metatarsal shaft and neck are treated the same way as nondisplaced zone 1 injury. Weight-bearing is allowed if the pain has subsided. For all fractures with delayed union or nonunion, surgery is advised. If the displacement is more than 3 mm or angulation more than 10?, the fracture is reduced and splinted. If follow up X-rays show that the fracture is still present, then percutaneous pinning or plate and screw fixation via surgery is considered.
All martial artists who undergo surgery with intramedullary screw fixation or bone grafting are made to wear a short leg cast for six weeks. Or they may be put in a plaster splint for 6 weeks. Both these options require bed rest with no weight-bearing. After 6 weeks, a gradual return to sport is permitted, as tolerated.
Home
The majority of acute MTP fractures are treated with conservative treatment. They heal by 6 to 8 weeks.
Diaphyseal stress fractures require up to 20 weeks for complete healing. Weight-bearing restrictions are important. Return to play is only allowed after there is radiographic evidence of complete healing.
Emergency
The initial treatment for most toe injuries regardless of grade is basic RICE therapy (rest, ice, compression, and elevation). Wear a stiff sole shoe or rocker bottom sole to limit motion. In severe injuries, a controlled ankle motion (CAM) boot or walking cast is advised. This limits motion at the joint. By minimizing motion, the plantar plate is allowed to heal. If the injury is stable, motion is allowed.
Medical
Grade 1 injuries heal in two weeks with conservative treatment. The martial artist can return to play as tolerated.
Grade 2 injuries require 4 to 6 weeks to heal. Martial artists are taped as they return to play as tolerated. After the acute phase, once the swelling is ended, the taping must provide resistance to hyper-extending the MTP joint. Corticosteroid and/or anesthetic injections are not prescribed.
Grade 3 injuries are severe but conservative treatment is chosen for a longer duration. This includes immobilization with a CAM boot. Another alternative is a short-leg walking cast for 4 to 6. After the initial immobilization, progressive, gentle range of motion is permitted. Some doctors will allow protected ambulation with modified shoe wear. The martial artist can also wear inserts of carbon-fiber or a foot-plate extension. The progression of activity is allowed as per the tolerance of the fighter. This injury takes 6 to 12 months to heal.
Surgery is an option if conservative management has failed. Unstable joints, capsular avulsion injuries, deformities, cartilage injuries, loose bodies, and sesamoid fractures are some reasons surgery is considered.
Surgical alternatives are medial plantar incision. Here, surgeons will attempt the direct repair of soft tissue injury.
Home
Physical therapy is very important when it comes to the treatment of turf toe. It starts with gentle passive motion at 7 to 10 days. The foot is usually non-weight bearing in a removable splint or boot. The toe is protected for 4 weeks. After 4 weeks, active motion is increased. Ambulation in the boot is allowed. The martial artists are asked to wear a modified shoe at 2 months. They are allowed contact activity. However, the toe needs to be protected from excessive dorsiflexion at 3 to 4 months. It takes about 6 to 12 months for a full recovery. Avoid steroid injections.
Emergency
The injury must be thoroughly cleaned with minimal debridement of both the nail bed and nail root. A doctor will reposition and anatomically repair significantly disrupted nail beds and nail roots. If this is not done accurately and immediately, nailbed growth is affected leading to deformed nails. Close approximation of the nail bed preserves the skin folds surrounding the nail margins. Any adhesions between the eponychium, nail bed, and root are prevented by replacing the nail or gauze packing to maintain the space.
Medical
Even if there is partial nail avulsion or the surrounding nail fold has been disrupted, then nail has to be removed. If there are associated lacerations of the nail bed blunt removal of the nail is necessary. The nail bed is then closed with absorbable sutures. The nail is replaced to allow new nail growth and the nail fold space is maintained with gauze packing.
Home
Some doctors may just apply Vaseline gauze after repair and allow it to separate on its own. A plaster volar splint rounded at the end can protect the toe-tip. Elevate the toe and check the injury in three days with a dressing change. Sutures in the nail or the gauze packing under the eponychium are removed in two weeks.
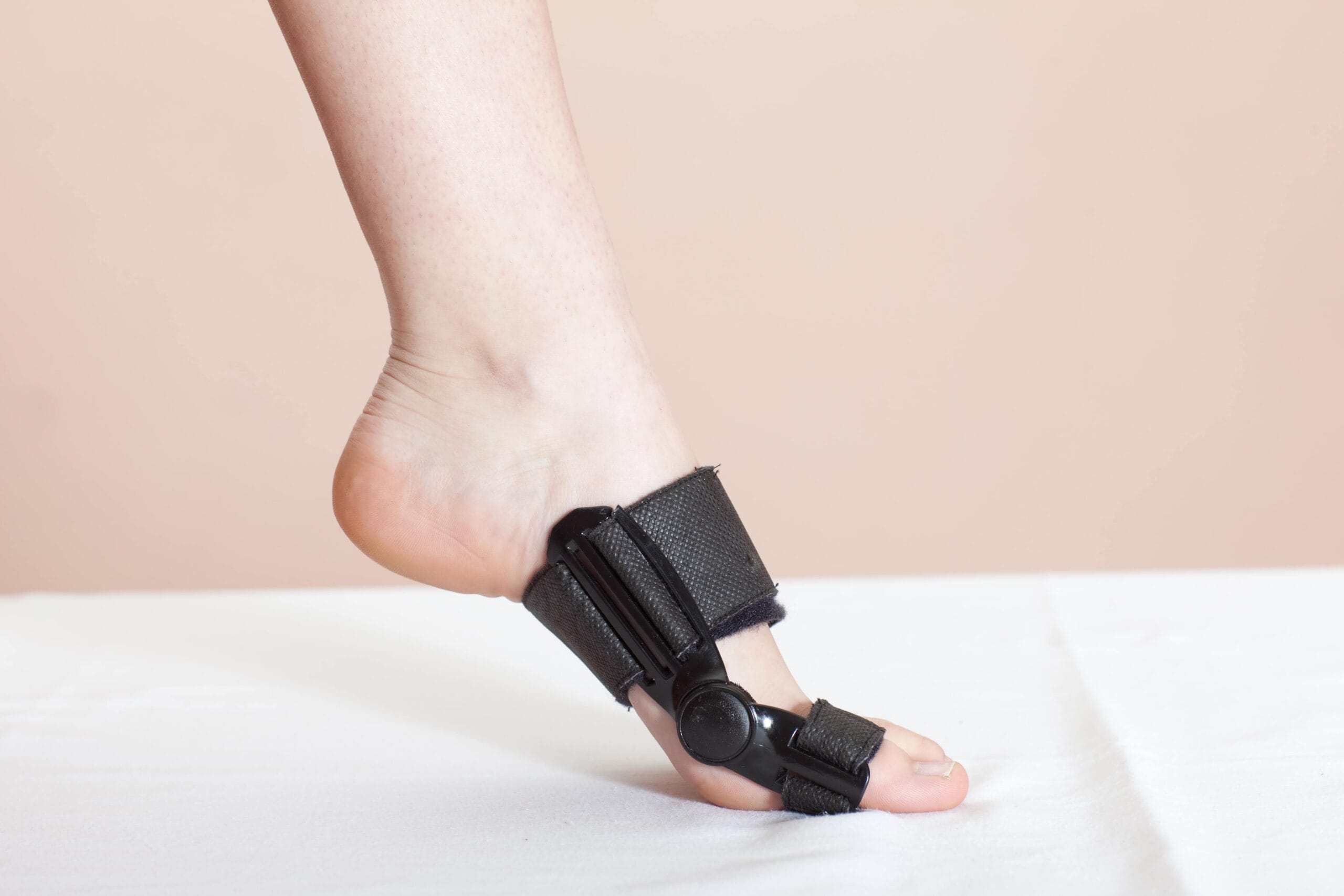
Common Treatments
Our Common Treatments section talks about how various therapies are used to treat lacerations and contusions affecting the toe.
