Combat Arts Hip Injuries Overview
Dustin “The Diamond” Poirier had to cancel his fight with Nate Diaz at UFC 230 in Madison Square Garden because of ongoing hip pain. “I do not have to have surgery,” Poirier said on Twitter. “I’m going to stay in Los Angeles and get stem cell injections in my hip on Monday. From that point, I will have a three-week recovery. After that, I will be able to go back to training 100 percent.”

The hips are the crucial center where weight and dan tien (point of internal power about two inches below the navel) give power and speed to kicks, strikes, turns, throws and support back strength.
“The martial arts are the No. 1 cause of injuries to the knee and hip, particularly amongst older athletes such as those in their 30s and 40s,” Dr. Klapper said. “I am seeing an epidemic of hip replacements, especially in those over 50.”
The good news is there really are extremely successful and efficient options now for hip injuries which range from simple home remedies, stem cell treatments, and other approaches, all the way to hip replacement surgery.
Many martial artists including senseis, shifus, masters, and practitioners doing karate, kung fu, jiu-jitsu, Muay Thai, and others have had serious hip injuries that required hip replacements and are still practicing, in some cases, more powerfully and intensely than they’ve been able to do in years.
It helps to find doctors such as Dr. Steve Mora who specialize in MMA and sports-related injuries and issues and treat athletes such as UFC champions Michael Bisping, TJ Dillashaw, and Tony Ferguson.
Dr. Mora says hip issues, pain, and injuries in Mixed Martial Arts (MMA) fighters are common since “combat athletes are unique in that their sport requires mastering various techniques which in turn predisposes them to various types of injury mechanisms. The successful MMA athlete has to practice boxing, Jujitsu, Muay Thai, wrestling, judo, kickboxing, along with ground and pound. Those in the combat arts train hard and are exposed to both acute trauma and cumulative training related trauma.”
Hip Injury Causes
High kicks, and particularly powerful roundhouse kicks, are the most common culprits for causing hip injuries. Dr. Mora says a correct diagnosis is essential for healing as many results from such varied actions as impact trauma, repetitive kicking and pivoting, overtraining, guarding on back resulting in hyperflexion / rotation, impact on groin or thigh from kicks or takedowns, lateral hip impacts from throws or takedowns resulting in landing on the side, tendonitis or arthritis.
One issue for martial artists with hip issues is the tendency to ignore pain. “Athletes wait too long to seek help for a potential injury because of the no-pain-no-gain ethic of some martial arts,” Dr. Klapper says. “Successfully treating your body is about listening to it on a daily basis, not waiting for it to shout.”



Hip Injury Symptoms
Dr. Klapper says that recognizing the signs of an injury is essential. “Athletes come to me when they are having pain in or around their hips and point to one of three areas: their groin, their side hip area (the pocket), or their buttock. Groin pain means damage to the hip, the pocket means it is bursitis or tendonitis, and the buttock indicates the injury is to the lower spine.”
Types of Hip Injuries
Cumulative trauma and acute trauma are common for those in the combat arts. They tend to practice a variety of techniques like boxing, jiu-jitsu, kicking, and grappling. All these moves involve the hip joints. Blocking kicks, guarding, and punching tend to also exert force on the hips. So many forces act on it like acute trauma, repetitive pivoting on a leg during a kick, hyperflexion of the hips, rotation, and lateral hip impactions injury when a fighter falls on his side.
Some of the injuries seen in those in the combat arts involve hip include Pubalgia, Heterotopic Ossification, Impingement of the hip, and hip fractures.
Hip Problems Are Common as You Age
Need Stronger Hip Muscles? We Can Help.
Related Injuries
Overview
This is a stress injury of the pubic symphysis. Repetitive use in MMA can cause microtrauma or injure the pelvic muscles. This causes an imbalance between the anterior muscles and the adductor muscles. As a result, the distribution of force across the pubic symphysis alters the joint. Eventually, the pubic bone is damaged and the cartilage is destroyed. Pubalgia is commonly seen in MMA that involves kicking. Often, a hernia is suspected and so pubalgia is not diagnosed immediately.
Symptoms
Causes
Athletic pubalgia is common among those in the combat arts who kick repeatedly or have lots of kicking maneuvers. This is a soft tissue injury of the abdominal muscles such as rectus sheath or pelvic muscles such as the adductors. MMA involves planting the feet and twisting with maximally. This exertion can tear the soft tissue of the lower abdomen or groin.
To learn how Pubalgia is diagnosed Click Here
This usually occurs due to a single traumatic event like a punch or kick to the hip area. A hematoma or a deep bruise ensues. For reasons unknown, the hematoma calcifies and ossifies. This is common in those in the combat arts because it only occurs in an area where frequent direct trauma is encountered.
It usually occurs 3 to 12 weeks after sudden trauma to the hip. However, it can take up to 6 months to present. A sudden kick or punch in the hip area can cause a hematoma to develop. Instead of healing, the hematoma calcifies. This happens frequently in those in the combat arts due to the repetitive injury or kicks in the hip area.
To learn how Heterotopic Ossification are diagnosed Click Here
The jiu-jitsu sage John Danaher who was the architect of UFC champions Georges St-Pierre and Chris Weidman has been plagued by Femoroacetabular Impingement (FAI). He admits the MRI of his hip looks like a car wreck and worse, he feels like he’s 100 with all the pain. The hip pain is secondary to mechanical impingement from an abnormal hip structure involving the femur and acetabulum. When an impingement occurs the femoral cam or bump collides with the acetabular rim. It results in the labrum and cartilage getting pinched. Over time, this causes the cartilage of the labrum to wear. Progressively, it leads to hip osteoarthritis if left untreated with repeated trauma.
As the hip rotates to extreme arcs of motion or if there is repetitive, abnormal contact between the bony prominences of the hip and femur, the soft tissue of the femoroacetabular joint gets damaged. The abnormal pathology includes the cam deformity of the femoral head-neck junction as well as pincer lesions of the acetabulum. They both contribute to impingement and pain. Any labral tears and or impingement of the hip causes abnormal gliding of the ball and socket mechanism of the hip joint. The joint tries to adapt, albeit painfully. Mixed Martial Arts fighters subject themselves to repetitive flexion and outward motion of the leg stressing the joint. They have pain when they flex and rotate the hip especially while guarding or checking a kick, if hip impingement is present.
To learn how Impingement of the hip is diagnosed Click Here
Hip injuries are common among those in the combat arts; they are due to acute injuries and more due to chronic injuries. The constant kicking and pivoting, checking, and guarding on one leg tends to stress the joint. Increased wear and tear cause the cartilage to wear off and the head of the femur to grind on the hip socket. The bone on bone contact gradually worsens in time and develops stress fractures. An acute injury like a sudden fall can also fracture the hip. Hip throws are common moves in MMA and are frequently used. At 35 Ben Askren, one of the most successful grapplers to grace martial arts retired as he needed a complete hip replacement due to years of training.
Hip fractures occur in those in the combat arts who withstand high energy trauma. They could be due to overuse of the hip joint through hip throws and pivoting movements of the hip or they could be due to an acute fall or injury. If the hip fracture also involves the fracture of the femoral neck then it will involve months of crutch use.
To learn how Hip Fractures are diagnosed Click Here
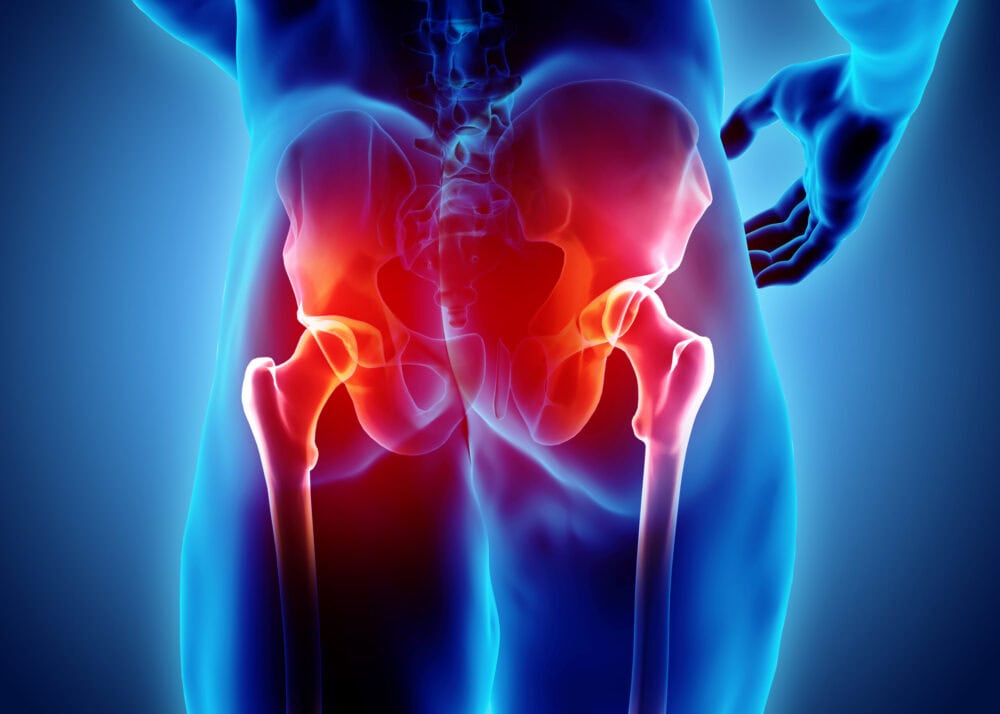


Common Injuries
Read more about hip injuries such as contusions and sprains in our Common Injuries section.
Hip Injury Diagnosis
Hip injuries require a variety of tests to confirm and diagnose them. Apart from imaging, neurological tests, gait tests, and ROM tests, are done to understand how the injury is affecting the body. Some are done clinically while the vast majority of hip injuries will require imaging modalities to rule out more complex pathology.
Injury Specific Diagnosis
Physical Exam
The doctor will start palpating laterally at the inguinal ligament and work to the pubic tubercle. The public symphysis is also checked. Any tenderness at or just above the pubic tubercle is indicative of pubalgia. Pain can also be elicited with resisted sit-up exams and hip flexion. In the resisted sit up exam, the fighter lies supine, with the feet stabilized. The arms are held straight ahead and a sit-up is done, holding for 5 seconds. If there is pain at the rectus sheath, the test is positive.
Valsalva maneuvers can also occasionally reproduce pain. Single or Bilateral Resisted Leg Adduction test is another diagnostic test for pubalgia. In this test, the fighter lies supine and flexes the leg to 30°. The doctor places his hand on the inner side of the heel and asks the fighter to resist abduction. If there is pain on flexion and extension, or any pain at all, the test is considered positive.
A sensory exam is done as sensory deficits and paresthesia in the lower abdomen, inguinal region, thigh, and genitals suggest entrapment of the iliohypogastric, ilioinguinal, and genitofemoral nerves.
Both hips are checked for a range of motion. To rule out isolated intra and extra-articular pathology, tests such as FADIR, FABER or Patrick Test, Scour, DEXRIT (Dynamic External Rotatory Impingement Test), and DIRIT (Dynamic Internal Rotatory Impingement Test).
Imaging
Radiographic must include a standing anteroposterior (AP) pelvis and lateral hip views. Doctors will look for intra-articular pathologies like arthritis, loose bodies, and acetabular dysplasia. Extra-articular pathology like pelvic avulsion fractures sustained during a fight or workout is also seen. Magnetic resonance imaging (MRI) of the pelvis is done in athletic pubalgia. A dedicated hip MR arthrogram is done if there’s a suspicion of labral tears. Rectus disruptions are seen as a cleft sign and tears are characteristics for pubalgia.
Lab Tests
Blood tests do not help confirm pubalgia. However, diagnostic intra- and extra-articular injections of local anesthetic and/or corticosteroid can also diagnose pubalgia. Doctors do it with a fluoroscope or with an ultrasound. After the injection of the hip joint, a provocation test is done to differentiate hip pain from pelvic pain. Any persistent pain in the adductor regions, despite an intra-articular injection, is diagnostic for pubalgia.
To learn how Pubalgia is treated Click Here
During the physical exam doctors look for local edema, effusion, erythema, warmth, and tenderness either in the tissue or joint. Fighters may also present with a low-grade fever and localized swelling. On neurological exam, they may demonstrate some spasticity near the affected joint.
Plain film radiographs will reveal circumferential bone formation around or near the affected joint. X-ray is specific for HO. Plain films don’t catch this until 3 to 4 weeks. Therefore, the triple-phase bone scan is preferred instead. A bone scan reveals this injury as early as 2.5 weeks.
CT scan delineates the area of bone formation before surgery. Other imaging like ultrasound and 3-dimensional stereolithography is also done, but not always necessary.
Blood tests are important for the diagnosis of HO. Alkaline phosphatase is the most commonly ordered lab test. It is not always elevated early on as the HO forms. It could take up to 2 weeks to rise. When it does, it climbs to 3.5 times the normal value 10-weeks after the injury. Serum alkaline phosphatase of more than 250 is also seen in HO. It does not indicate the severity of the disease. If the fighter has other long bone injuries, then the alkaline phosphatase is raised.
Erythrocyte sedimentation rate (ESR) is another inflammatory marker that is tested for HO. It is not specific but ESR greater than 35 mm/hr can indicate its development. C-reactive protein is a non-specific inflammatory marker that is elevated in early HO. Creatine kinase (CK) determines the severity of HO but is not a very specific test and can demonstrate resistance to standard etidronate treatment.
To learn how Heterotopic Ossification are treated Click Here
Doctors will look for pain radiating to the thigh. They will check for the "C sign." It is formed by the index finger and thumb over the anterolateral area of the hip.
They will observe the gait, hip range of motion, and strength. The Trendelenburg gait or abductor lurch is tested. It indicates abductor muscle weakness. While testing hip range of motion, decreased hip flexion and internal rotation is a sign of positive impingement. Pain with hip flexion at 90⁰, adduction, and internal rotation is another positive sign. The FABER test (hip Flexion, Abduction, and External Rotation) is positive for labral tears. They will check for any audible snapping of the hip. Palpable snapping with the hip range of motion indicates another syndrome that must be differentiated from FAI.
Evaluation of the hip with plain films is the first step. X-rays must include a standing anterior-posterior (AP) pelvis, AP hip and lateral of the hip. These views assess the pelvis and femur. Standing films are necessary despite the pain as they offer the hip position while it’s at a functional load-bearing position.
It also detects hip dysplasia if present. Cam and pincer lesions can be seen in X-ray views. The lateral center edge angle (LCEA) is measured to assess for hip dysplasia with Xrays. Pincer deformities appear as excess bony growth along the acetabular edge. A cam deformity appears as an excess bony growth along the femoral head-neck junction. The head may not be spherical anymore.
Other views include the false profile and the Dunn views of the hip. Here the fighter stands at an angle of 65 degrees as the X-ray is directed towards the affected hip.
The Dunn view is a lateral view of the affected hip. It is obtained at a 45⁰ angle to the hip. It best assesses the cam deformity.
Magnetic resonance imaging (MRI), with or without intra-articular contrast injection, also assesses FAI. It is helpful as it is very informative about potential labral or cartilage injury resulting from impingement. The MRI provides 3D images of the bony structure and impingement cysts in the femoral neck if any. It can also identify other sources of hip pain such as avascular necrosis, stress fractures, bursitis, and tendonitis.
Blood tests are not needed to diagnose this injury. However, in preparation for surgery, blood tests are required. This includes a complete blood count, type, and Rh for potential transfusions, PT, PTT, and basic metabolic panel.
To learn how Impingement of the hip is treated Click Here
The physical examination is done to check for pain, mobility through ROM testing, and any potential limb deformity. If the leg is shortened and externally rotated limb then it aids in the diagnosis. This occurs due to the unopposed pull of the iliopsoas muscle. Any pain while palpating the groin, axial loading of the hip and 'pin-rolling' of the leg is suspicious for a hip fracture.
Doctors will perform a full primary trauma and secondary trauma assessment.
Hip fractures are diagnosed on plain film radiographs. An anteroposterior and lateral view of the pelvis is done. A lateral view of the affected hip is also done. MRI can pick up occult hip fractures missed on plain films and, therefore is the gold standard. CT is an alternative when an MRI is not available.
Intracapsular hip fractures are classified with the Pauwel classification. This classification divides fractures into three groups:
Type 1: <30 degree
Type 2: 31-50 degrees
Type 3: >50 degrees
An increased angle is a more unstable fracture. Their healing will take longer.
The Garden classification is used for intracapsular hip fractures. It has four fracture patterns:
Type 1: incomplete fracture and no displacement
Type 2: complete fracture and no displacement
Type 3: complete fracture and partial displacement
Type 4: complete fracture and complete displacement
Extracapsular fractures are divided into trochanteric and subtrochanteric fractures. Extracapsular fractures are divided by the AO classification:
A1: two-part, stable fracture
A2: comminuted, unstable fracture
A3: reverse or transverse, unstable fracture
Different fracture types dictate the surgical treatment a fighter will receive.
Fighters must have blood tests to assess for anemia, renal function, and coagulation profile. A bone screen is done to assess osteoporosis or calcium abnormalities. A cross-match is done as operative management for fractured hips can cause significant blood loss.
To learn how Hip Fractures are treated Click Here
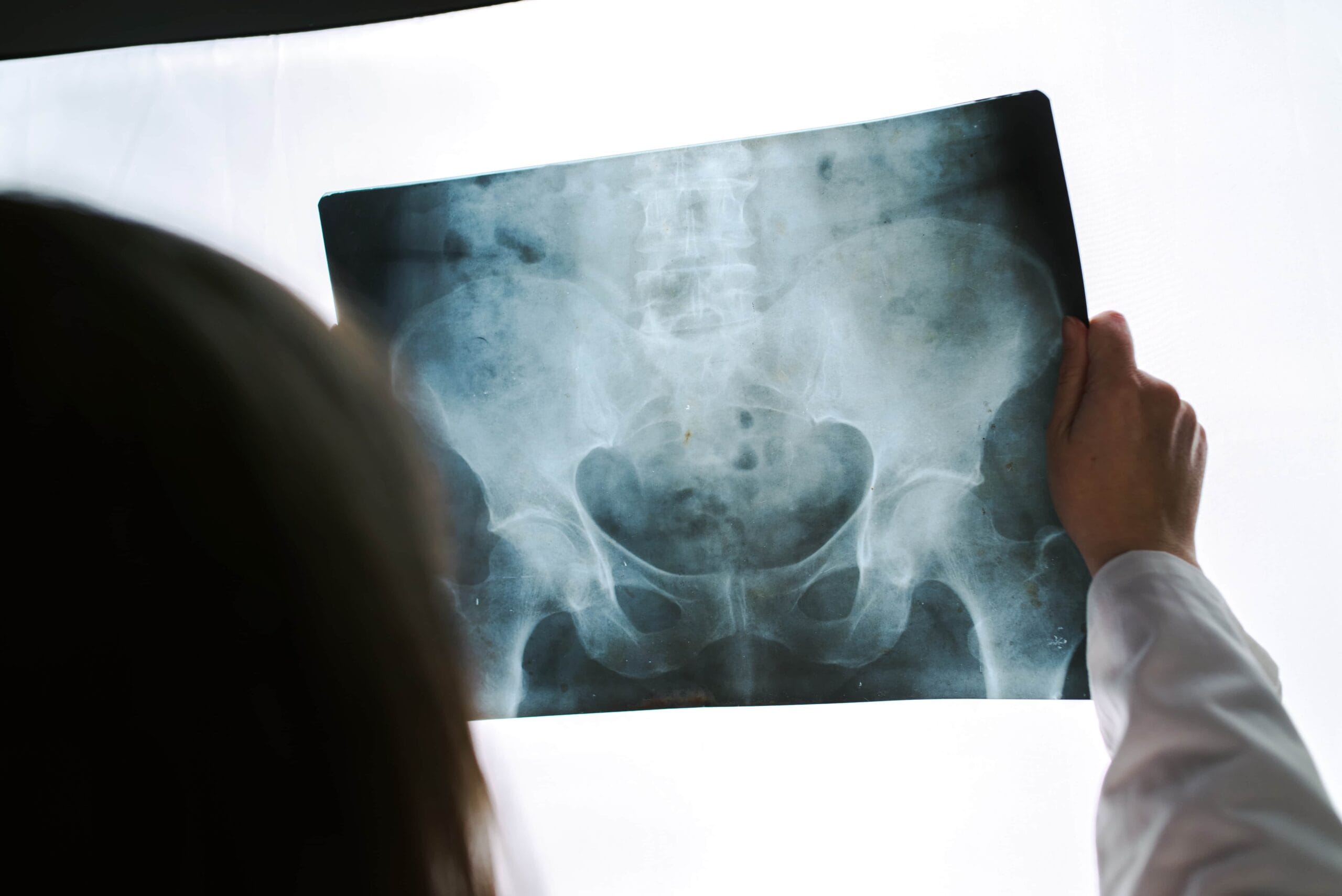


Common Diagnoses
Read our Common Diagnoses section to find out how various tests and imaging modalities are used to diagnose hip injuries.
Hip Injury Treatment
The treatment for hip injuries depends on the type of injury, the location, and the mechanism. Rest, ice, and pain management form the key for acute injuries. However, when it comes to the hip joint, surgery is the absolute treatment.
Injury Specific Treatment
Emergency
Initially, 7 to10 days after the injury, rest and ice should suffice. Any bulge in the groin, compression, or a wrap may relieve pain. This must be confirmed by a doctor.
Medical
Rehabilitation with physical therapy is the best therapy for athletes with athletic pubalgia. However, this treatment is tailored based on the level of the athlete. Physical therapy includes core strengthening and stabilization, restoration of pelvic tilt, and postural training. Avoid overload the hip with an increasing range of motion especially those with hip pathology. Conservative treatment is done for 3 months. If it fails to relieve symptoms, surgery is advised. For those athletes who are training for competitive sports, a trial 4-week period of rest is done. For pain management, nonsteroidal anti-inflammatories and oral steroid tapering treatment are tried.
Selective corticosteroid or platelet-rich plasma injections into the rectus muscle and/or adductor longus muscle is also done. If symptoms ease then, the fighter can return to the sport through a trial period. If pain persists, it is up to the fighter to decide to rest or cross over to surgical treatment.
Surgical treatment includes laparoscopic and open procedures. During these operations, the posterior wall is reinforced and the conjoint tendon or the rectus sheath is fixed. If adductor pain is present, then adductor tenotomy is advised. This is where the tendon is divided. A full return to sport can be made in about 6–8 weeks if it is an isolated athletic pubalgia repair. If another hip pathology exists, then expect healing to take about 4 months.
Home
Stop training, get the weight off the injured hip, and either begin R.I.C.E. treatment if the injury is mild or find a doctor or go to the hospital if the injury is intensely painful and/or critical. Acupuncture, CBD oil, different types of stem cell, massage, hydrotherapy, yoga, and tai chi are all proven treatments. Traditional Chinese medicine, and Ayurveda which is a therapy that originated in India, are both useful treatments. Deep Tissue Laser Therapy may be used for decreasing pain and inflammation.
Physical therapy must be started two weeks after sustaining the injury. The focus is on improving strength and flexibility in the abdominal and inner thigh muscles.
Usually, post injury, the development of HO is never suspected. It takes weeks for this injury to develop. However, rest and ice are advised to prevent any further aggravation of the hematoma and to allow its complete healing.
The first step in the treatment of HO is mobilization with ROM exercises and pain management with indomethacin. Etidronate therapy and surgical resection are advised if the initial treatment doesn’t work. Early passive range of motion exercises must start once HO is diagnosed. This is to prevent ankylosing of joints.
Surgical resection of mature bone is absolute treatment. It is done only once the HO is fully matured. This is about 12 to 18 months after the initial injury.
Indomethacin and etidronate are prescribed to arrest bone formation in HO. Rofecoxib 25 mg per day for 4 weeks or indomethacin 75 mg daily for 3 weeks is also prescribed for pain management.
The best therapy for HO is preventative. This is done by gentle ROM exercises, indomethacin, etidronate, and external beam radiation. Indomethacin is commonly used for prophylaxis. Other NSAIDs include meloxicam, celecoxib, rofecoxib, and ibuprofen.
Etidronate is a bisphosphonate to prevent heterotopic ossification. They are specifically used if there are spinal cord injuries.
If an acute injury is present, the first step is still medical treatment. These are tried for a period to allow the injury to heal. Pain management with NSAIDS and steroids are advised.
The treatment for impingement of the hip is both medical and surgical. Medical alternatives include physical therapy, modifying activity, and pain medication. This is typically done with NSAID’s. Intraarticular injection with local anesthetic and steroid is advised if the pain is unbearable. This is a diagnostic and therapeutic tool. It confirms the location of the pain. If all these measures fail, then surgery is advised.
In surgery, the bony causes of impingement are resected and the soft tissues are repaired. Surgery is done arthroscopically or in an open technique. For cam lesions involving the femoral head-neck junction, a cam resection or femoral osteoplasty is done. Surgeons use a high-speed burr and shave down the excess bone.
Pincer lesions on the acetabulum are repaired by an acetabular osteoplasty. For labral tears, the labrum is repaired or simply debrided. If there is focal cartilage damage, a microfracture is made to stimulate new cartilage growth.
Hip dysplasia if any is surgically treated by a pelvic osteotomy. The periacetabular osteotomy is commonly done by reorienting the acetabulum. Osteoplasty of the femur and pelvis is done by open surgical dislocation of the hip. However, hip arthroscopy is now preferred as the soft tissue is less disturbed. Open surgical dislocation requires extensive soft tissue dissection and longer recovery time. Despite its advantages, hip arthroscopy is preferred.
Fighters who undergo surgery for FAI have a rehabilitation protocol. Avoid weight-bearing status for 2 to 6 weeks. Protected weight bearing is advised to prevent stress on the osteoplasty of the acetabulum and to protect the repaired labrum.
Physical therapy is started early. It begins with a passive range of motion exercises of the hip for the first 3 to 4 weeks. Weight-bearing is advanced. It is followed by an active range of motion four weeks after surgery.
After 4 to 8 weeks, strengthening exercises and gait training can begin. Between 8 to 12 weeks, therapists will stress on the recovery of complete hip strength, core strength, balance, and proprioception. After 12 weeks, they will add flexibility exercises like jogging, jumping, and agility exercises.
In the emergency department, ATLS treatment must begin. Fighters can lose up to 1 liter of blood from proximal femoral fractures. This bleeding is internal and therefore occult. Fluid replacement and blood transfusion must be done early.
Avoid preoperative fasting for too long. Fasting causes hypoglycemia, immunosuppression, and dehydration. It also promotes catabolism. It is recommended that fighters fast from fluids for 2 hours and from food for 6 hours before surgery.
Oral or intravenous analgesics are given. If pain control is not achieved, a fascia-iliac nerve block is used. Do not apply limb traction, or attempt to reduce this injury even if the injury or fall was witnessed ringside.
The treatment depends on the location of the fracture. Most fighters are operated within 48 hours.
Intracapsular Fractures can be dangerous since the vessels that supply the joint capsule can be damaged. They result in avascular necrosis of the femoral head.
The arthroplasty preferred for displaced intracapsular hip fractures is a total hip replacement (THR) or a hemiarthroplasty. For younger athletes, open reduction and internal fixation of displaced intracapsular hip fractures are considered.
Undisplaced intracapsular fractures are managed conservatively or surgically. Surgical options include fixation or arthroplasty. Fixation is thought to be preferred to arthroplasty as it preserves the native joint. Mobility and function are better. A sliding hip screw (SHS) or cannulated hip screws (CHS) are two such fixation techniques.
After surgery, protected weight-bearing is allowed to prevent fracture displacement. In arthroplasty, the risk of avascular necrosis is removed. This risk persists in those undergoing fixation.
In extracapsular fractures, fixation is the treatment of choice with intramedullary nails (IMN) and sliding hip screws (SHS).
After surgery, blood transfusion is recommended if the hemoglobin is below 8 g/dL. Blood transfusion is also done if there are symptoms of anemia like pallor and breathlessness. It is important to mobilize early. Those fighters undergoing arthroplasty can move immediately without weight restrictions. For those undergoing fixation, protected weight-bearing is advised to prevent any displacement of the fracture.
Regular intensive physiotherapy is advised to restore full mobility. Return to play is debatable and depends on the surgery and the recovery time.



Common Treatments
Go through our Common Treatments section to find out how various therapies are used to treat injuries of the hip joint.
